Loss of consciousness may be caused by syncope (the patient usually recovers within a minute) or may signal the onset of coma. Altered mental status: see Impaired Consciousness.
Basic ManagementTop
1. Evaluate the patient using the ABCD scheme. Basic life support: see Cardiac Arrest. Assess the patient’s response to verbal and tactile stimuli. If the pulse is absent, begin cardiopulmonary resuscitation (CPR). If available, ask a bystander to call for help (or if in hospital, consider activating the emergency response team). Advanced life support: see Cardiac Arrest.
2. Clear the airway (see Cardiac Arrest; in trauma patients, particularly after head or neck injury, do not tilt the head backwards or in other directions), administer 100% oxygen via a face mask, check the capillary blood glucose level, and establish a peripheral IV line.
3. Monitor the vital signs. If blood pressure is low, administer 1 L crystalloid solution (eg, 0.9% NaCl) or, if not available, elevate the lower limbs to 45 degrees.
4. If the loss of consciousness is a result of trauma or a head or neck injury is suspected, stabilize the cervical spine (apply a rigid cervical collar if available) and carry out a rapid trauma survey.
5. Protect the patient from environmental extremes. If the loss of consciousness may have been caused by external factors (eg, hyperthermia, hypothermia, or gas poisoning [most frequently carbon monoxide]), and it is safe for you to do so, remove the patient from the environment (transferring a nontrauma patient: Figure 1). If the patient is already in hospital, ensure he or she is moved to an area capable of providing appropriate support.
6. If the loss of consciousness (in a nontrauma patient) is prolonged but the patient is hemodynamically stable (heart rate, blood pressure, and respiratory rate are within normal limits), you may place the patient in the recovery position (see Figure 6 in Cardiac Arrest).
7. If the patient does not regain consciousness, continue the management you have already initiated. Call for advanced help as required, depending on the patient’s requirements as well as your level of expertise and comfort (eg, unstable arrhythmia, refractory hypotension, a persistent Glasgow Coma Scale score <8 [see Table: Glasgow Coma Scale]), and investigate for causes of coma (see Table 1 in Coma).
8. If the patient recovers rapidly, investigate for causes of the transient loss of consciousness.
FiguresTop
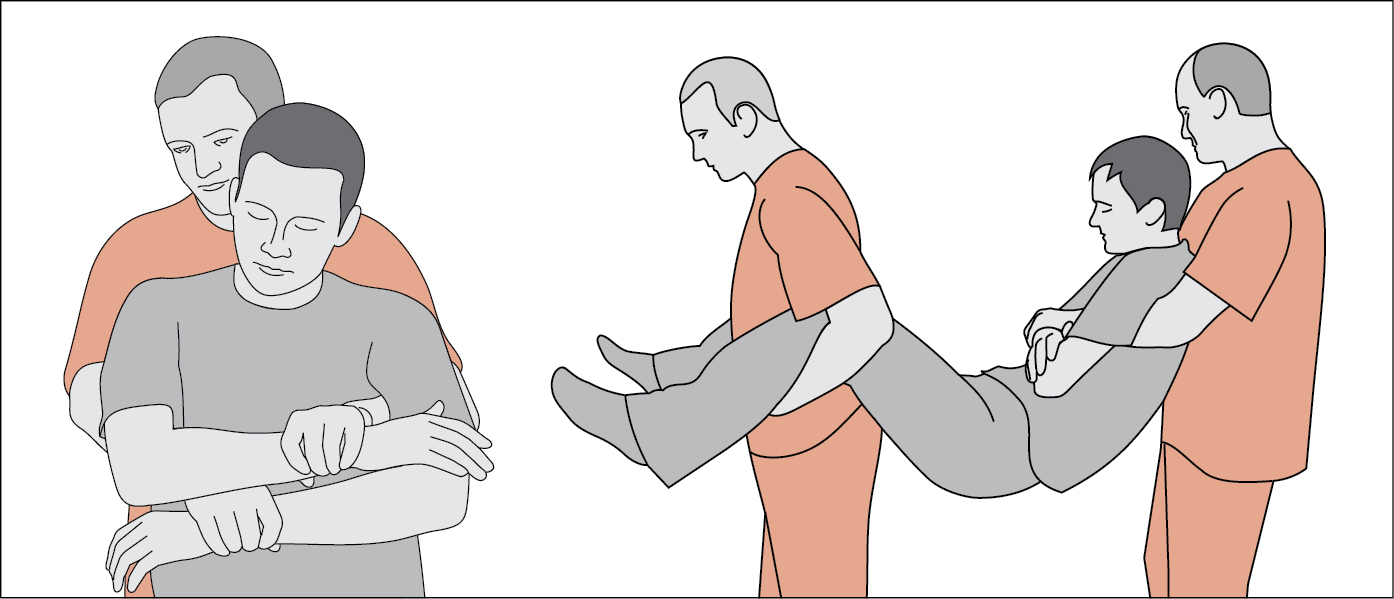
Figure 1.3-1. Safe transfer of an unconscious nontrauma patient by 2 persons.