Definition and EtiologyTop
Lymphedema is a condition characterized by swelling primarily in the subcutaneous tissue that results from lymph stasis caused by either congenital defects or acquired damage to the lymphatic vessels. This impaired lymphatic flow leads to chronic inflammation, which can vary in severity, eventually causing hypertrophy (thickening) of the skin and subcutaneous tissue.
Lymphedema can be categorized as either primary or secondary. Primary lymphedema arises due to inherent abnormalities in the lymphatic vessels, often stemming from a congenital or inherited condition. Secondary lymphedema, which is more common, occurs when the lymphatic system is damaged due to other diseases or medical treatments. Detailed classification and causes: Table 3.13-1.
Clinical FeaturesTop
Secondary lymphedema (eg, following lymphadenectomy or infection) usually develops after a few months or even years of a latency period. Initially it presents as pitting edema but typically hardens and becomes nonpitting with time due to fibrosis. Lymphedema usually begins distally and progresses proximally. However, in patients with damage to the proximal lymphatic system, lymphedema may affect only the proximal portion of an extremity and an adjacent quadrant of the trunk (eg, arm and/or breast lymphedema following lymphadenectomy due to breast cancer, thigh and/or external genitalia lymphedema after lymphadenectomy due to urogenital or gynecologic cancer; Figure 3.13-1). Depending on the cause, lymphedema may be unilateral or bilateral.
Progression of lower limb lymphedema eventually causes massive edema of the dorsum of the feet (Buffalo hump sign) and swelling of the toes (squaring toes sign). Hardening of the skin of the forefoot causes inability to pinch and lift the skin at the base of the second toe (Stemmer sign).
Clinical stages of lymphedema based on the International Society of Lymphology (ISL) system:
– Stage 0: Impaired lymph flow without visible edema.
– Stage 1: Edema resolves after limb elevation or overnight rest.
– Stage 2: Edema does not resolve completely after limb elevation.
– Stage 3: Sustained edema with trophic skin changes and deformation of the limb.
DiagnosisTop
In the majority of cases diagnosis is based on clinical manifestations. If necessary, perform lymphoscintigraphy. Ultrasonography, magnetic resonance imaging (T2-weighted MRI), computed tomography (CT), or radioactive isotope studies may be useful in diagnosis.
Differential diagnosis includes lipedema (mostly in women; symmetric accumulation of fat in the legs sparing the feet [“column-like legs”]), edema due to chronic venous insufficiency, positional edema as a result of prolonged sitting or standing in individuals without venous insufficiency, myxedema in patients with hypothyroidism, pretibial myxedema in patients with Graves disease, idiopathic cyclic edema, edema in patients with advanced heart failure or hypoalbuminemia, enlargement of the limbs due to tumors, postthrombotic syndrome, and limb hypertrophy.
TreatmentTop
The key treatment method is comprehensive therapy consisting of skin and wound care, compression therapy, and lymphatic drainage using decompression exercises and massage-like techniques by physiotherapists. Patients should also be advised on maintaining ideal body weight, limb elevation, and avoiding prolonged limb placement in a gravity-dependent position. Exercise is generally safe and should be allowed with compression garments. Compression therapy is highly recommended using compression bandages, compression garments, and intermittent pneumatic compression.
In addition to good skin hygiene and avoidance of injuries, chronic suppressive antibiotic therapy for several months or years may be warranted to prevent recurrent infection (clinical experience only). Common regimens include IM benzathine penicillin G (INN benzathine benzylpenicillin) 1.2 million IU every 2 to 4 weeks for prevention of beta-hemolytic streptococcal infection and oral trimethoprim/sulfamethoxazole double strength bid for prevention of staphylococcal infection. Some other regimens include erythromycin or cephalexin.
In patients not responding to compression therapy, surgical intervention such as liposuction, lymphatic bypass procedures, and vascularized lymph node transfer can be helpful. Contraindications to surgery include acute cellulitis, recent deep vein thrombosis of the lower limbs, and decompensated congestive heart failure.
ComplicationsTop
1. Recurrent infections (eg, cellulitis, lymphangitis, and tinea pedis in between toes).
2. Disfiguration of the affected limb and elephantiasis.
3. Recurrent and difficult to treat ulcers of the affected limbs, mostly legs.
4. Colonization with bacteria and fungi resulting in chronic malodorous limbs.
5. Elephantiasis nostras verrucosa presenting as thick verrucous changes on top of fibrotic changes of legs.
6. Reduced limb function in severe cases.
Tables and FiguresTop
|
Primary lymphedema |
Secondary or acquired lymphedema |
|
– Lymphedema congenita presenting at birth or during infancy – Lymphedema praecox, the most common type of primary lymphedema presenting around puberty and affecting predominantly legs – Lymphedema tarda presenting in adulthood, usually at the age of 35 years |
– Infections, particularly parasitic (eg, filariasis) – Recurrent skin infections (eg, cellulitis) – Post surgical treatment (eg, following mastectomy or lymph node dissection in breast cancer [Figure 1] or in melanoma) – Post radiotherapy for cancer – Related to malignancy due to obstruction of lymphatic vessels by neoplasm (eg, ovarian and peritoneal cancers) or due to extensive involvement of lymph nodes by malignancy (lymphoma) – Lymphedema due to extensive involvement of lymph nodes by granulomatous process (eg, sarcoidosis) – Posttraumatic lymphedema – Postinflammatory lymphedema (complication of arthritis, vasculitis, or lymphadenitis) – Combined venous and lymphatic edema in patients with chronic venous insufficiency – Idiopathic lymphedema – Lymphedema associated with morbid obesity |
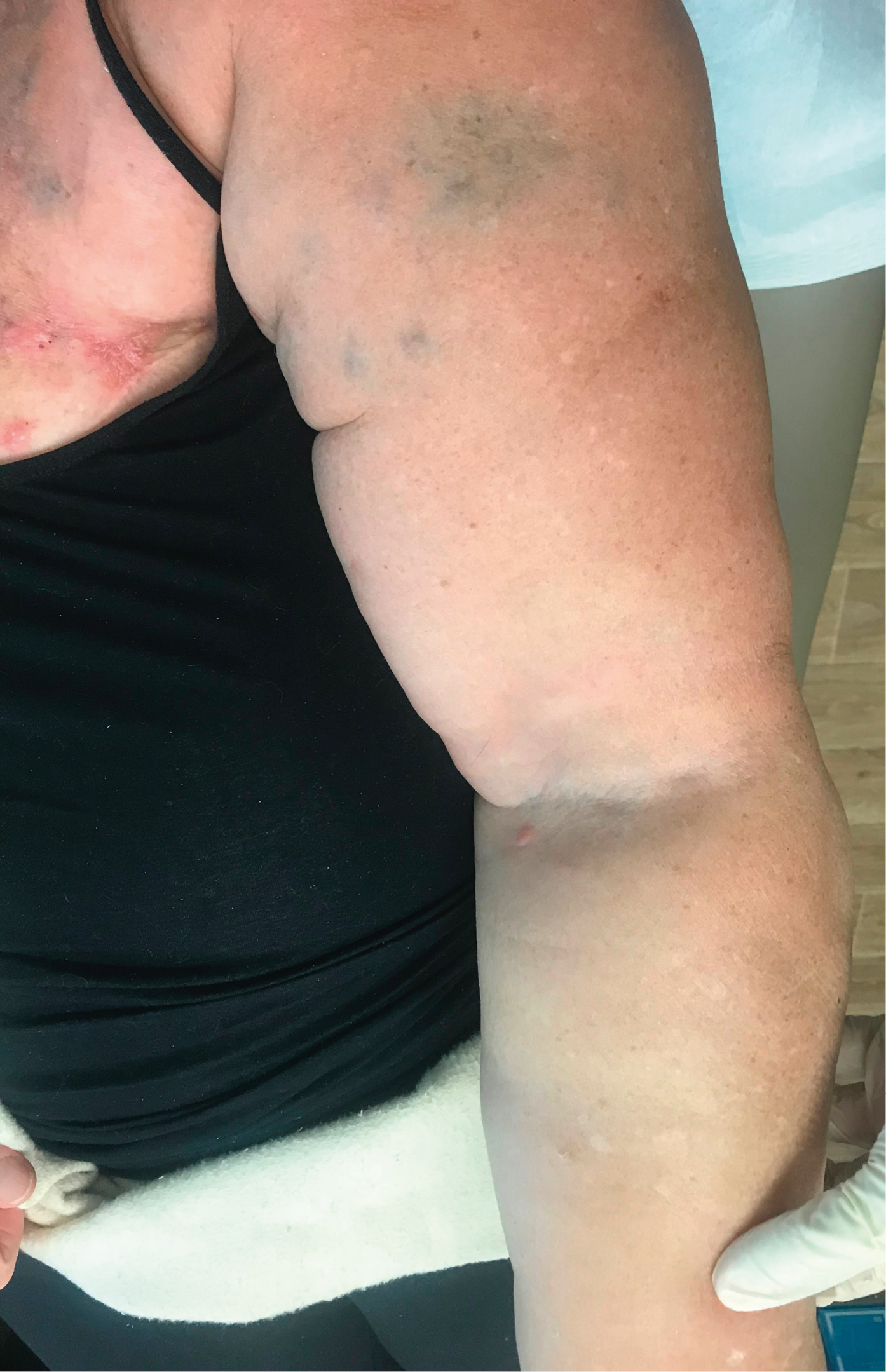
Figure 3.13-1. Lymphedema of the left arm 7 years after left breast cancer mastectomy and left axillary lymph node dissection.