Definition, Etiology, PathogenesisTop
Serum sickness is a reversible systemic reaction due to the formation of immune complexes with a foreign antigen present in circulation (type III hypersensitivity reaction).
“Classic” serum sickness results from the formation of immune complexes due to immunization of a human host with a foreign protein. Serum sickness–like reactions refer to a constellation of symptoms clinically resembling classic serum sickness but typically caused by drugs, and less frequently by infection. The pathogenesis of these reactions is not understood.
Causes:
1) Serum sickness:
a) Foreign proteins: Equine diphtheria antitoxin, botulinum antitoxin, rabies antitoxin, snake antivenom, antithymocyte immunoglobulin (rabbit), chimeric monoclonal antibodies (eg, rituximab, infliximab), streptokinase.
b) Case reports have implicated humanized monoclonal antibodies, allogenic human plasma, insect stings, mosquito salivary protein, vaccinations, and allergen immunotherapy extracts.
2) Serum sickness–like reactions:
a) Drugs: Most commonly antibiotics—specifically penicillin, amoxicillin, cefaclor, and sulfamethoxazole/trimethoprim—although a wide range of medications have been implicated.
b) Viral infections, for example, acute hepatitis B.
Clinical Features and Natural HistoryTop
Signs and symptoms typically start 7 to 14 days after exposure to the causative agent, though they can occur earlier on subsequent exposures. They last between 1 and 2 weeks and resolve spontaneously, provided the offending exposure has been removed. Typical symptoms include:
1) Fever: Fever occurs in virtually all patients and is typically >38.5 degrees Celsius. In serum sickness–like reactions, it tends to be present but less severe.
2) Dermatologic findings: Approximately 95% of patients have a pruritic rash, which is most commonly urticarial but can be macular erythematous, papular, or morbilliform. The rash is typically symmetric and does not involve the mucous membranes. Initially, the rash is present on the hands, feet, and trunk (Figure 1) but later may spread to the whole body. If the antigen was injected subcutaneously or intramuscularly, the first signs may appear at the injection site. When urticarial lesions appear, they may be atypical in that they last longer than 24 hours. Other possible dermatologic findings include small-vessel vasculitis involving the skin, lesions suggestive of erythema multiforme (sparing the mucous membranes), palmar erythema, and atypical maculopapular lesions located on lateral surfaces of fingers and toes or following a ribbon-like pattern along the external surfaces of the soles.
3) Other symptoms: Joint pain and tenderness, edema and erythema of the periarticular area (rare), muscle pain, lymphadenopathy and splenomegaly (in 10%-20% of patients; rare in serum sickness–like reactions), edema of the lips and eyelids, nausea, vomiting, abdominal cramps, diarrhea, headache and visual disturbances, peripheral neuropathy, neuritis, nephritis, meningitis and encephalitis, Guillain-Barré syndrome, myocarditis and pericarditis, dyspnea.
DiagnosisTop
Diagnosis is based on a characteristic pattern of signs and symptoms associated with exposure to a probable causative agent.
1. Blood tests: No abnormalities are specific to serum sickness. Frequent findings include elevated erythrocyte sedimentation rate and C-reactive protein levels, lymphocytosis, eosinophilia, transient elevation of alanine aminotransferase and aspartate aminotransferase levels, low levels of C3 and C4 complement components, low levels of total hemolytic complement activity (CH50), and elevated levels of circulating immune complexes (elevated levels of immune complexes and low levels of C3 or C4 are rarely observed in serum sickness–like reactions).
2. Urinalysis: Proteinuria, hyaline casts, and erythrocytes in the sediment.
3. Histologic examination of skin biopsy material (performed only in case of diagnostic difficulties): Leukocytoclastic angiitis, deposits of immunoglobulins and C3 in the vessel walls.
Rash associated with viral infections, arthritis (including rheumatic fever), polymyositis or dermatomyositis, erythema multiforme, angioedema, urticarial vasculitis, systemic vasculitis, drug reactions with eosinophilia and systemic symptoms.
TreatmentTop
There are no evidence-based guidelines or high-quality controlled trials on which to base therapy. The general approach is as follows:
1) Discontinue the drug causing the reaction.
2) Symptomatic management:
a) Use antihistamines for relief of pruritus.
b) Use nonsteroidal anti-inflammatory drugs for relief of joint symptoms.
In patients with severe arthritis, high fever, or severe generalized rash, short courses of systemic glucocorticoids may be used. A typical approach would be oral prednisone 0.5 to 1 mg/kg once daily, with dose tapering to discontinuation over 1 to 2 weeks.
Symptoms typically resolve in 1 to 2 weeks once the offending trigger has been removed but can persist for months in a minority of cases. Long-term sequelae are uncommon.
PreventionTop
The suspected trigger should be avoided. If the use of the drug suspected of causing serum sickness is indispensable, antihistamines and systemic glucocorticoids can be coadministered.
FiguresTop
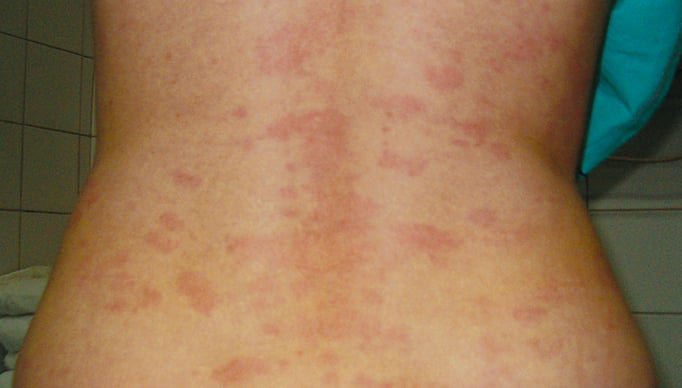
Figure 2.6-1. Skin lesions in serum sickness.