Etiology and PathogenesisTop
1. Etiologic agent: Human itch mite, Sarcoptes scabiei variant hominis.
2. Pathogenesis: The entire life cycle of the parasite is in the epidermis. The parasite can penetrate the skin in all life stages; gravid females make a permanent burrow in the epidermis to lay eggs. Larvae hatch after ~50 hours and reach adulthood within ~2 weeks. In classic scabies infestation, typically 10 to 12 adult female mites are living in the epidermis, with the numbers being higher in crusted scabies. The signs and symptoms are caused by the presence of mites in the epidermis and by the host’s immune response. S scabiei antigens are strong allergens and elicit pronounced cell-mediated immune response (type IV hypersensitivity reaction). The majority of skin manifestations associated with scabies derive from a sensitization reaction.
3. Reservoir and transmission: The only reservoir is humans. Infestation spreads through direct skin-to-skin contact with an affected individual, including sexual contacts. Crusted scabies is also transmitted through contact with contaminated upholstered furniture, bed linens, and toys (in classic scabies infestation through contact with contaminated objects is controversial).
4. Incubation and contagious period: In individuals with initial infestation, the incubation period is 3 to 6 weeks from infestation. Reinfestations become symptomatic within several days. Scabies is contagious for the entire duration of the infestation.
EpidemiologyTop
Scabies is prevalent worldwide, but it is most common in tropical and subtropical climates, where up to 50% of the populations are affected. In resource-poor communities children and young adults are the most affected group. In high-income countries infestations are also observed in elderly individuals with immunodeficiency. Transmission occurs mainly in crowded sites (eg, in daycare centers, preschools, boarding schools, orphanages, nursing homes, hospitals). Endemic infestations are observed in densely populated areas, particularly among populations with low economic status.
Clinical Features and Natural HistoryTop
The cardinal feature is pruritus, which intensifies with an increase in body temperature, eg, at night after covering the body. Pruritus disturbs nocturnal sleep and causes irritability and fatigue. This, in turn, may affect daily activity and the effectiveness of work or learning processes.
Skin lesions:
1) Scabetic burrows: Characteristic tracks in the epidermis, several millimeters in length (Figure 10.9-1), primarily on lateral digital surface, in skin folds, and on buttocks. Burrows may be difficult to find and are sometimes visualized following the application of weak iodine solution on the affected skin.
2) Eczematous lesions: Numerous disseminated papules, edematous papules, crusts, erosions, and excoriations caused by scratching. The interscapular area, head, soles, and palms of the hand are spared. In men itchy nodules may appear on the scrotum and penis. In women nipples are frequently involved.
The signs and symptoms are particularly pronounced in persons with poor hygiene, immunosuppressed individuals, or persons with atopic dermatitis. Several types of scabies are distinguished, depending on the patient’s age and immunity status:
1) Pediatric scabies: Plantar and palmar lesions are common; the scalp may also be affected. Pustular, vesicular, and nodular reactions are more common in young children.
2) Geriatric scabies: Skin lesions may be less severe due to weaker immune response. Pruritus may not correspond to the extension of skin lesions. Skin of the head may also be involved.
3) Nodular scabies manifests with purple or brownish firm nodules (Figure 10.9-2). Typical locations include the scrotum, buttocks, and skin folds. The nodules develop as a sensitization reaction to S scabiei. They are characterized by intense itching but do not contain the parasite. They persist long after completion of curative treatment.
4) Bullous scabies resembles bullous pemphigoid and affects primarily the elderly. Bullous scabies manifests as numerous small vesicles and erosions that mimic bullous disease.
5) Crusted scabies (Figure 10.9-3) is particularly common in immunocompromised patients, individuals with psychiatric disorders, and neglected and bedridden persons. The host’s compromised immune response allows for a very intense multiplication of the parasite. The large numbers of S scabiei colonizing the epidermis lead to hyperkeratosis, with thick scaly plaques and hypertrophic papillous eruptions. Systemic erythroderma may develop. Crusted scabies involves the skin of the entire body, and pruritus is mild or absent. Untreated scabies may persist for long periods and does not resolve spontaneously.
DiagnosisTop
1. Identification of the etiologic agent: Microscopic examination of the epidermis. Parasites in skin scrapings can be visualized under the microscope, but a negative result does not exclude scabies. The use of a dermoscope may increase the number of microscopy-positive results.
2. Other tests: Eosinophilia and elevated serum IgE levels are found in some patients.
Diagnosis is based on the patient’s history and typical clinical features, preferably with a positive result of microscopic examination of skin scrapings. If the patient has typical clinical manifestations, introduce antiscabetic treatment even if the microscopic result is negative.
Diffuse eczema (regardless of etiology), atopic dermatitis, drug-induced reaction, dermatitis herpetiformis (Duhring disease), papular urticaria, nodular prurigo, senile pruritus and pruritus secondary to systemic diseases; bullous pemphigoid (for bullous scabies); psoriasis, Darier disease, severe seborrheic dermatitis, and other conditions that cause erythroderma (for crusted scabies); borrelial lymphocytoma (for nodular scabies).
TreatmentTop
1. Scabicides should be used after a >10-minute bath, as this improves the drug’s penetration through the skin. They are applied thoroughly to all areas of the body from the jawline down, with particular attention paid to skin folds, interdigital spaces, perigenital areas, and spaces under the fingernails. In the elderly and in young children, scabicides should also be used on the head, avoiding the eyes and mouth. All of the patient’s household contacts and sexual partners should be simultaneously treated, irrespective of their symptoms.
2. Scabicides for topical use:
1) Permethrin cream (5%) or gel (4%): First-line treatment due to its efficacy (>95%) and safety profile. It kills adult mites and larvae by paralyzing their nervous system. Permethrin products are applied once for 8 to 10 hours and then washed off. If removed earlier (eg, after washing the hands), reapplication is recommended. Recommended amounts for a single application: Adults, 30 g; children aged 6 to 12 years, 15 g; children aged 2 months to 5 years, 7.5 g. The treatment can be repeated after 7 to 14 days.
2) Benzyl benzoate lotion (10%): Demonstrates antiscabetic and antibacterial activity. The lotion should be thoroughly rubbed into the skin in all areas of the body (including the scalp, if needed), except for the face, once daily, preferably in the evening. Repeat the application for 3 to 4 days, without washing the skin. Wash the body after completing the treatment. The product is not suitable for young children. A 10% lotion can be used in children aged >2 years.
3) Crotamiton cream or lotion (10%): Demonstrates antiscabetic (60% efficacy) and antipruritic activity. The drug is absorbed through the skin and excreted with urine, but it is characterized by low toxicity to humans. The product should be rubbed into the skin once daily for 3 to 5 days without washing the body. Bathing is recommended 2 days after completion of treatment. The product should not be applied on the face or damaged skin. It needs to be used with caution in sensitive areas (skin folds, scrotum). The drug is approved for use in children aged >1 year. In young children 1 application may be enough for full curative effect.
4) Sulfur ointment (6%-10%): Contains sulfur and salicylic acid suspended in a lipid medium (petrolatum). The product is considered very safe and can be used in pregnant patients and small children. It is applied for 3 to 5 days without washing the skin. Bathing is recommended after completion of treatment. The treatment can be repeated after 2 weeks.
Oral ivermectin in a single dose of 150 to 200 microg/kg; the treatment can be repeated after 2 weeks if needed.
1. Standard therapy is usually insufficient. There is no universally accepted treatment regimen for crusted scabies. A hot >10-minute bath or application of softening or keratolytic agents (eg, urea) is recommended prior to initiation of the therapy to soften the thick scales.
2. Depending on the severity of infestation, use one of the following:
1) Permethrin (5%) applied twice for 12 hours and washed off after the second application. Repeat the procedure after 7 days.
2) Permethrin (5%) applied twice for 12 hours and washed off after the second application, followed by crotamiton for 6 days and, again, followed by 5% permethrin.
3) Permethrin cream (5%) and ivermectin 200 microg/kg.
4) Permethrin cream (5%) applied every 2 to 3 days for 1 to 2 weeks and ivermectin in 3 doses (on day 1, 2, and 8), in 5 doses (on day 1, 2, 8, 9, and 15), or in 7 doses (an additional dose on day 22 and 29).
3. After completion of treatment:
1) Consider the use of sulfur ointment for several days.
2) Perform a follow-up examination of skin scrapings from 3 areas; if the result is positive, repeat the therapy until the curative effect is achieved.
3) Other recommendations for patients:
a) All towels, bed linens, blankets, and coverlets should be changed and washed.
b) Clothes worn by the patient over the last week should be washed at >60 degrees Celsius or ironed.
c) Items that cannot be washed (footwear, soft toys) should be placed in airtight foil packaging for 72 hours at room temperature or frozen at –20 degrees Celsius for 12 hours.
d) Carpets and upholstered furniture should be thoroughly vacuum-cleaned (parasite-destroying detergents can be used).
e) The procedures above can be abandoned for items that have not been used over the last week.
Management of Postscabies Pruritus
To manage postscabies pruritus, which may persist for up to several weeks, consider:
1) Emollients: Pruritus that persists after completion of treatment may be caused by irritation and dryness of the skin.
2) Topical formulations with glucocorticoids.
3) Antihistamines, in particular, first-generation, demonstrating a sedative effect.
4) Oral glucocorticoids for particularly persistent pruritus.
ComplicationsTop
1. Secondary bacterial infections: Staphylococcal or streptococcal, commonly manifesting as impetigo, multiple abscesses, pyoderma, or bacterial dermatitis or cellulitis. Bacterial infections secondary to scabies are a serious problem in tropical countries, where generalized infections and sepsis are common.
2. Nonpurulent complications of secondary bacterial infections: A significant problem in countries with a high prevalence of scabies. Streptococcal dermatitis secondary to scabies may lead to poststreptococcal glomerulonephritis; its links with rheumatic fever are unclear.
Special ConsiderationsTop
Since scabicides are applied on large body surface, there are concerns that significant amounts of the drugs may get into bloodstream and affect the development of the fetus. No reliable evidence is available on the safety of scabies treatment in pregnant and breastfeeding patients. Sulfur ointment seems the safest option provided that it does not contain salicylic acid. Permethrin and 10% benzyl benzoate are category B drugs, which means they appear to be safe and there have been reports of their use in pregnant women with no adverse consequences for the fetus. Crotamiton is not indicated in pregnant patients (category C). Although the data are limited, it appears that permethrin (single application), benzyl benzoate (2 applications), and sulfur ointment (3 applications) can be safely used both in pregnant and in breastfeeding patients.
Sulfur ointment seems the best solution for the treatment of children aged ≤2 months. Permethrin can be used in children aged >2 months. Crotamiton is approved as scabies treatment in children aged >1 year; however, it should be used with caution in young children. Crotamiton should not be applied on large areas, which virtually excludes its use in young children. A single application is recommended. A 10% benzyl benzoate is considered safe in children aged ≥2 years. No reliable evidence is available on the safety of ivermectin in children aged <5 years.
PrognosisTop
In most cases scabies responds well to treatment. Pruritus persisting after treatment completion is sometimes observed. Untreated scabies can continue for long periods and progress to crusted scabies. If there are no complications such as postinfectious glomerulonephritis or rheumatic fever due to secondary streptococcal infection, prognosis is very good. Reinfestations are possible if treatment was not used in household contacts and other close contacts of the patient.
PreventionTop
None.
1. Simultaneous treatment of all household contacts and other close contacts of the patients, including their sexual partners.
2. Disinfection of clothes and objects in the patient’s surroundings after completion of treatment.
3. For institutional infestations (eg, in preschools, daycare centers, hospitals): Treatment of employees.
FiguresTop
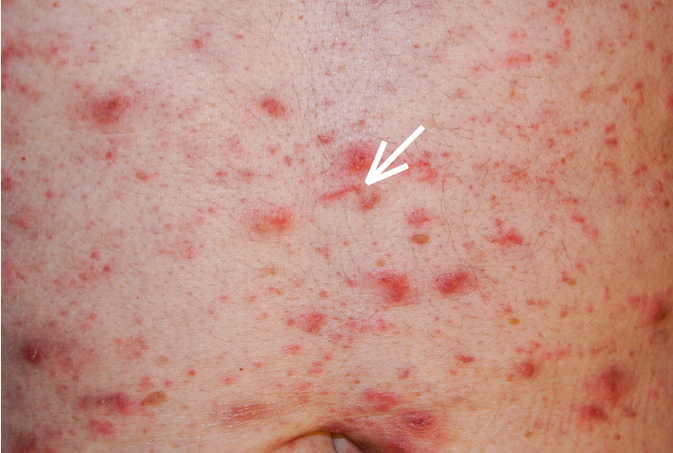
Figure 10.9-1.
Scabetic burrow visible at the center of the photograph, pointed by the arrow.
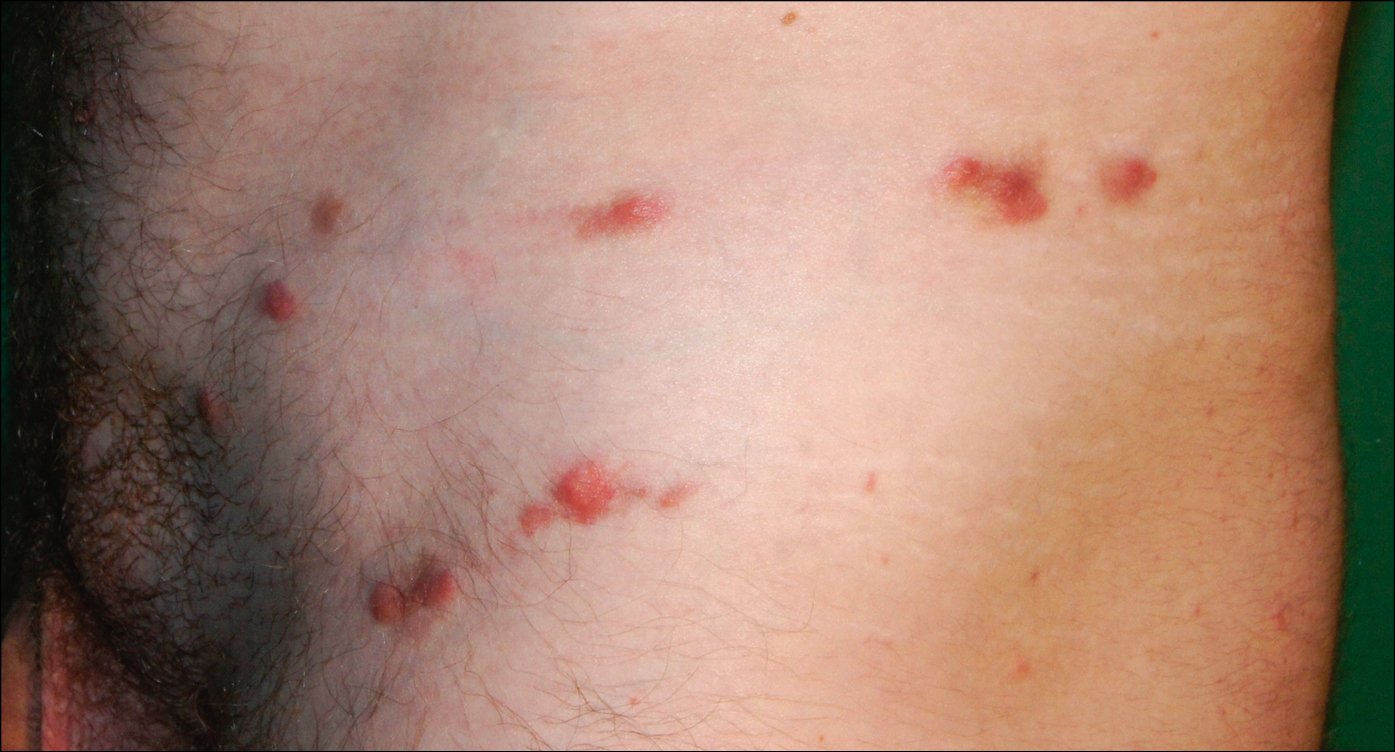
Figure 10.9-2.
Nodular scabies.
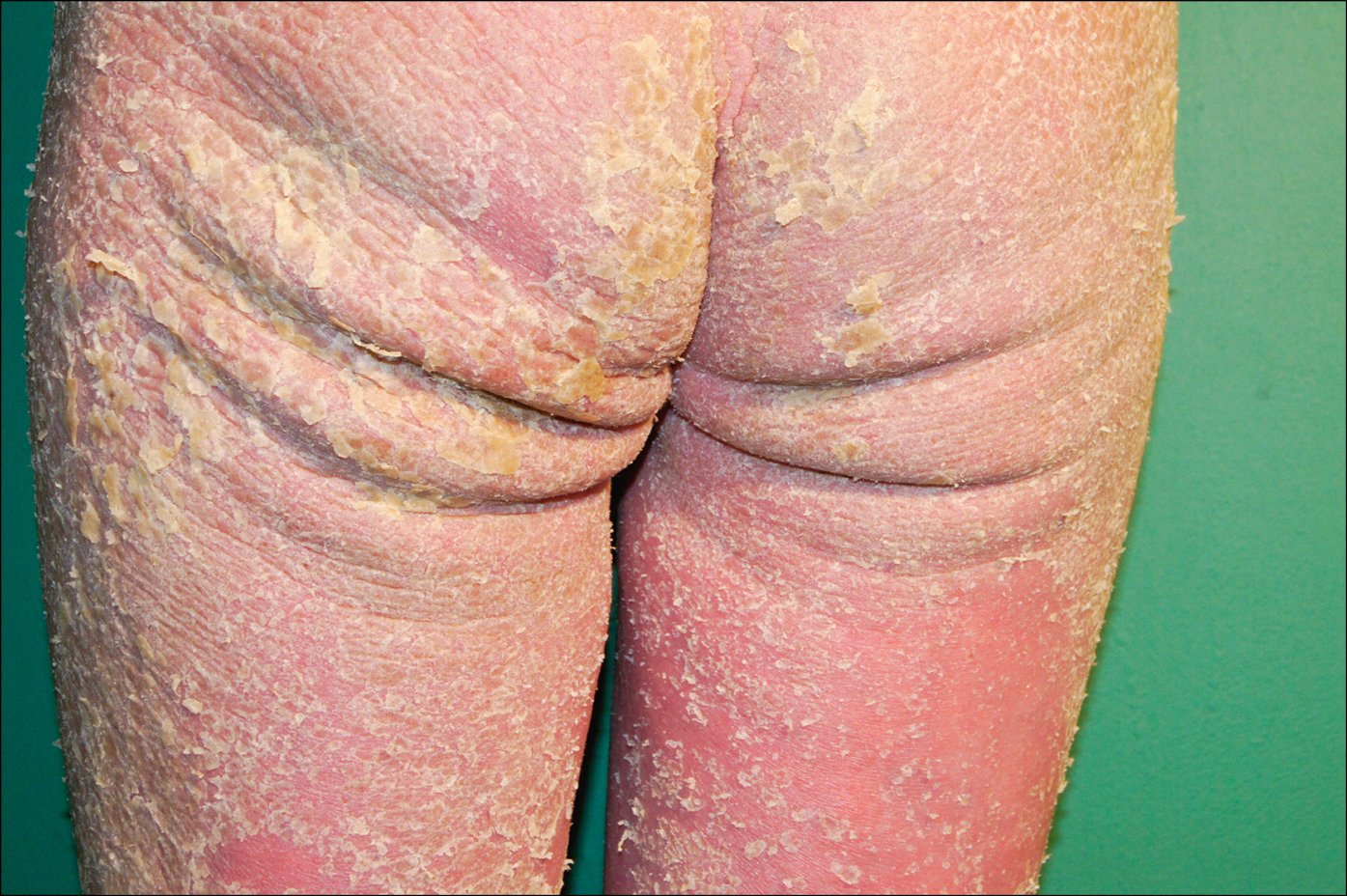
Figure 10.9-3.
Crusted scabies with visible erythroderma and pronounced hyperkeratosis.