Leung AK, Barankin B, Lam JM, Leong KF, Hon KL. Tinea pedis: an updated review. Drugs Context. 2023 Jun 29;12:2023-5-1. doi: 10.7573/dic.2023-5-1. PMID: 37415917; PMCID: PMC10321471.
Ohn J, Yu DA, Park H, Cho S, Mun JH. Green nail syndrome: Analysis of the association with onychomycosis. J Am Acad Dermatol. 2020 Sep;83(3):940-942. doi: 10.1016/j.jaad.2020.01.040. Epub 2020 Jan 28. PMID: 32004651.
Definition, Etiology, PathogenesisTop
Dermatophytes are fungal infections that affect keratinized structures, such as the epidermis, hair, and nails.
1. Etiologic agent: Dermatophytes of the Trichophyton, Microsporum, and Epidermophyton genera. Depending on the reservoir, the fungi can be divided into anthropophilic, zoophilic, and geophilic:
1) Anthropophilic dermatophytes (eg, Trichophyton rubrum, Trichophyton interdigitale, Trichophyton tonsurans, Microsporum audouinii) are well adapted to live in the human body and cause chronic infections with mild symptoms.
2) Zoophilic dermatophytes (eg, Microsporum canis, Trichophyton mentagrophytes, Trichophyton verrucosum) in humans cause infections that are usually associated with enhanced inflammatory reaction.
3) Geophilic dermatophytes (eg, Microsporum gypseum) live in soil and rarely cause infections in humans.
2. Reservoir and transmission: An individual may become infected through direct contact (tinea capitis in children) or indirect contact (foot mycosis—infection acquired at the swimming pool) with anthropophilic dermatophytes. Dermatophyte spores and mycelium fragments can survive in the external environment up to 18 months and become the source of infection. Infection with zoophilic dermatophytes is possible through contact with domestic animals (often in children) or farm animals (in farmers and veterinarians).
3. Risk factors:
1) Toenail onychomycosis: Nail injuries; increased nail plate curvature; increased sweating; immunosuppression; decreased blood supply to the foot due to atherosclerosis, diabetes, or advanced age.
2) Inguinal mycosis: Obesity; excessive sweating; wearing tight, nonbreathable clothes.
Clinical Features and Natural HistoryTop
1. Foot mycosis (tinea pedis, also known as athlete’s foot) and toenail onychomycosis.
Types of foot mycosis:
1) Interdigital: Lesions are initially located in the area between the toes. Gradually erythema and scaling subside and maceration and cracking of the epidermis are observed (Figure 10.8-1). The most common location of tinea pedis is between the fourth and fifth toes. In persisting infection, lesions extend peripherally from the interdigital spaces onto the surrounding skin on the dorsal and plantar foot surfaces. The eruptions are accompanied by pruritus.
2) Hyperkeratotic (“moccasin foot”): Lesions appear on the plantar and lateral side of the foot. Erythema, excessive keratinization, and exfoliation are observed. If the stratum corneum is markedly thickened, painful cracking may occur under the pressure of walking.
3) Vesiculobullous (inflammatory): Characteristic vesicles or blisters are initially located within the foot arch, and then spread onto the entire plantar area. Vesicles dry out or, if perforated, form oozing erosions.
Types of toenail onychomycosis:
1) Distal and lateral subungual onychomycosis: The most common form of dermatophyte onychomycosis. The infection starts at the distal edge of the nail plate and gradually spreads within the nail bed towards the proximal nail fold. The fungi cause keratinization of the nail bed, separation of the nail plate from the bed, and accumulation of subungual debris under the nail plate. This leads to discoloration of the nail, most often to a milky color (whitening of the nail [Figure 10.8-2]). Additionally, the space between the altered nail plate and bed may be inhabited by bacteria and molds. In such cases the color changes to yellow, green, or dark brown.
2) Proximal subungual onychomycosis: Infection starts in the proximal nail plate and whitening of the nail is observed.
3) White superficial onychomycosis: Infection of the superficial nail plate layers that presents with white spots on the nail surface.
4) Endonyx onychomycosis: A rare type of toenail onychomycosis, in which the dermatophyte mycelium grows through the nail plate but does not reach the nail bed. No brittle keratoid masses indicating nail bed infection are seen. The nail plate becomes discolored, dull, and brittle.
5) Dystrophic onychomycosis: An advanced form of onychomycosis with complete nail plate destruction.
2. Hand mycosis and fingernail onychomycosis: Dermatophyte infection of the hands and fingernails is very rare. In the majority of cases only one hand is affected, and the disease is most often accompanied by foot mycosis, as the infection is transferred from the feet to hands (Figure 10.8-2). Symptoms include hyperkeratosis and palmar peeling. When the infection spreads to the dorsal hand surface, erythematous lesions that are well separated from the healthy skin, with pronounced inflammation of the margins are observed. Nails are thickened, brittle, with uneven surface, and discolored (white or yellow).
3. Body mycosis (tinea corporis) (Figure 10.8-3): The infection presents with well-circumscribed, scaley, erythematous lesions. Inflammation is more evident on the margins and sometimes accompanied by blisters and pustules in an annular configuration, hence the common name “ring worm.” Fungal penetration to hair follicles may result in granulomatous reaction with the formation of papular lesions (Majocchi granuloma).
4. Facial mycosis (tinea faciei): This most often occurs in children. As in other dermatophyte infections, pronounced inflammation of the lesions is observed in an annular pattern (exacerbated on the margins and less severe in the central part) as well as superficial exfoliation. In some cases the picture may be less specific, and the nonexfoliating erythematous lesions may be similar to those observed in other dermatoses such as seborrheic dermatitis, atopic dermatitis, and lupus erythematosus.
5. Inguinal mycosis (tinea cruris): Dermatophyte infections of the groins are more common in adults. Lesions are located in the groins and the upper part of the inner thigh, classically sparing the scrotum (Figure 10.8-4). Exfoliating erythematous lesions with enhanced inflammation on the margins are observed.
6. Tinea capitis: This is more common in children. Microsporum infection is characterized by the presence of spores on the outer surface of hair (ectothrix infection). Hair shafts are broken at different heights. Involvement of other hair-bearing sites is also possible, such as within the beard (tinea barbae).
In the case of Trichophyton infection, spores are located both outside and inside hair shafts. The inside arrangement leads to shaft damage and breakage at the level of skin surface (black spots are visible). Skin lesions are erythematous, with more severe inflammation on the margins than in the center, and well separated from the healthy skin. In infections caused by zoophilic fungi (M canis), the inflammation is usually very severe and leads to formation of a boggy swelling with pustules on the surface (kerion celsi: see Figure 10.8-5).
In infection caused by anthropophilic fungi (M audouini, T tonsurans), minor peripherally spreading exfoliation is observed on the scalp. Anthropophilic fungi cause epidemics of tinea capitis in schools and kindergartens.
A different clinical course is observed in favus, an infection caused by Trichophyton schoenleinii, still found in the Middle East and Africa. Favus manifests with discs of mycelium and exfoliating epidermis tightly adhering to the skin surface and causing scarring.
DiagnosisTop
Dermatophytosis is diagnosed based on a positive result of a mycologic examination of scrapings from affected skin surface. In body mycosis, plaques located on the margins of the skin eruption are scrapped for analysis. In nail infections, nail clipping is done or scrapings are collected from under the nail plate. The collected material is used for direct microscopic examination with 10% KOH, and culture is started on Sabouraud medium. Culture results are obtained within ~3 weeks.
Dermatophytes can also be detected using polymerase chain reaction (PCR). Mycology laboratories may use both methods, classical (direct examination + culture) and molecular, as they are complementary.
1. Foot and hand mycosis: Contact dermatitis, dyshidrotic eczema, psoriasis.
2. Onychomycosis: Nail psoriasis, lichen planus, nail candidiasis.
3. Body mycosis: Nummular eczema, psoriasis.
4. Inguinal mycosis: Yeast and bacterial intertrigo, erythrasma, psoriasis.
TreatmentTop
1. Antifungal treatment:
1) In general topical treatment is sufficient. Use creams or ointments containing an antifungal agent for 6 weeks: azole derivatives (clotrimazole, miconazole, isoconazole, econazole, bifonazole, flutrimazole), allylamines (terbinafine, naftifine), ciclopirox.
2) Systemic treatment should be used if topical treatment is ineffective. Options:
a) Oral terbinafine 250 mg once a day for 2 to 6 weeks.
b) Oral itraconazole 200 mg bid for 7 days (100 mg once a day for 30 days in hyperkeratotic mycosis).
c) Oral fluconazole 150 mg once a week for 4 to 6 weeks.
2. Symptomatic treatment: In severe inflammation start treatment with application of a topical formulation containing an antifungal agent and glucocorticoid for 2 to 3 days.
1. Antifungal treatment:
1) Topical treatment (options):
a) Ciclopirox (nail enamel) for 6 to 12 months.
b) Amorolfine (nail enamel) for 6 to 12 months.
c) A combination cream product containing urea 40% and bifonazole: In stage 1 of treatment (7-14 days), the altered part of the nail plate is softened by urea and then removed; in stage 2 the patient continues treatment with bifonazole cream until regrowth of a healthy nail plate.
2) Systemic treatment should be used if multiple nails are involved and lesions appear on the entire nail plate. Options:
a) Oral terbinafine 250 mg once a day for 8 weeks in fingernail onychomycosis and for 12 weeks in toenail onychomycosis.
b) Pulse therapy with oral itraconazole 200 mg bid for 7 days; 2 pulses in fingernail onychomycosis, 3 pulses in toenail onychomycosis; 3-week interval between the pulses.
c) Oral fluconazole 150 mg once a week until regrowth of a healthy nail (3-6 months for fingernails, 6-12 months for toenails).
Oral and topical combination therapy is recommended. If there is no response to treatment, switch to a different oral drug after 6 months. If the patient is not responding again and the mycologic result remains positive, initiate terbinafine for 1 month or additionally administer a single pulse of itraconazole.
2. Surgical treatment: Surgery is indicated if systemic and topical treatment is ineffective. Consider chemical ablation or surgical removal of the nail plate (with concomitant therapy with oral terbinafine 250 mg once a day or oral itraconazole 200 mg once a day for 1 month). Surgical treatment is associated with risk of damage to the nail matrix and nail bed.
Body, Facial, and Inguinal Mycosis
Antifungal treatment:
1) Topical treatment is similar as in foot mycosis and usually lasts 2 to 3 weeks. Continuation of therapy for 1 to 2 weeks after symptom resolution is recommended.
2) Systemic treatment (options):
a) Oral fluconazole 150 mg once a week or 50 mg once a day for 2 to 4 weeks.
b) Oral itraconazole 200 mg once a day for 7 days or 100 mg once a day for 15 days.
c) Oral terbinafine 250 mg once a day for 2 to 4 weeks.
Antifungal treatment:
1) Systemic treatment (options):
a) Griseofulvin is particularly effective in infections caused by Microsporum fungi (eg, M canis); 20 to 25 mg/kg/d for 6 to 8 weeks.
b) Terbinafine is effective in infections caused by Trichophyton fungi (eg, T tonsurans); the recommended treatment duration for Trichophyton infection is 2 to 4 weeks, and for Microsporum, >4 weeks. In adults and children aged >2 years, the dose depends on body weight: <20 kg—62.5 mg/d; 20 to 40 kg—125 mg/d; >40 kg—250 mg/d.
c) Itraconazole is used in patients aged >16 years at a dose of 2 to 5 mg/kg of body weight/d for 4 to 6 weeks.
d) Fluconazole at a dose of 3 to 6 mg/kg of body weight/day in children for 6 to 8 weeks. If standard treatment is ineffective, it can be extended up to 12 to 16 weeks.
2) Adjuvant topical treatment: Use antifungal agents in the form of solutions, gels, or shampoos.
ComplicationsTop
Each type of toenail onychomycosis may lead to toenail dystrophy. Untreated favus may lead to extensive and irreversible hair loss.
PreventionTop
None available.
Prevention of toenail onychomycosis recurrence: After treatment completion patients should be instructed to disinfect shoes and socks with, for example, 10% formalin solution or 1% hydroxyquinoline sulfate/boric acid solution.
FiguresTop
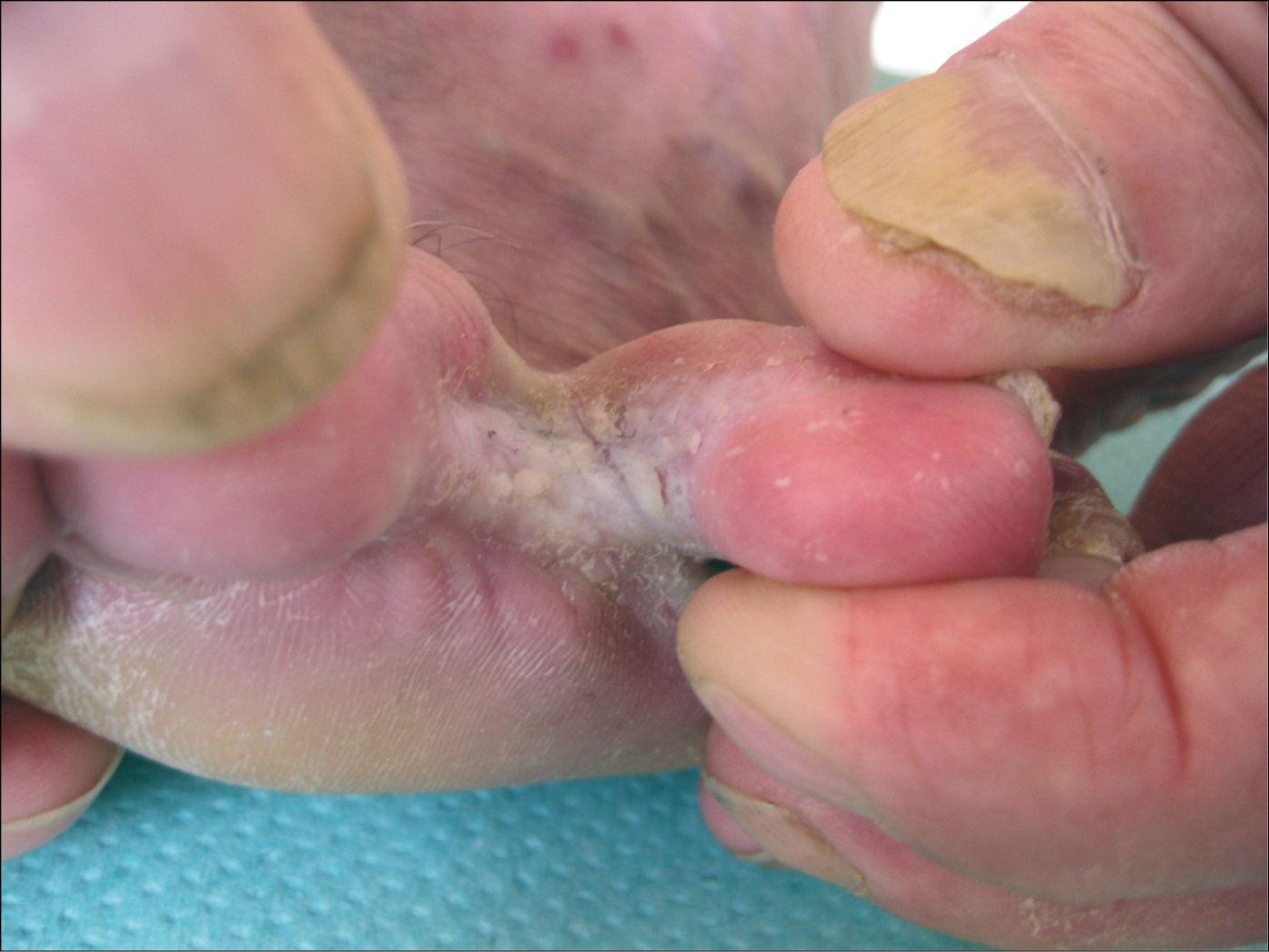
Figure 10.8-1. Interdigital foot mycosis. Maceration and scaling of the epidermis in the interdigital spaces. Secondary fingernail onychomycosis. Thickened, brittle nail plate of the thumb, keratinization of the nail bed, altered plate color (whitening).
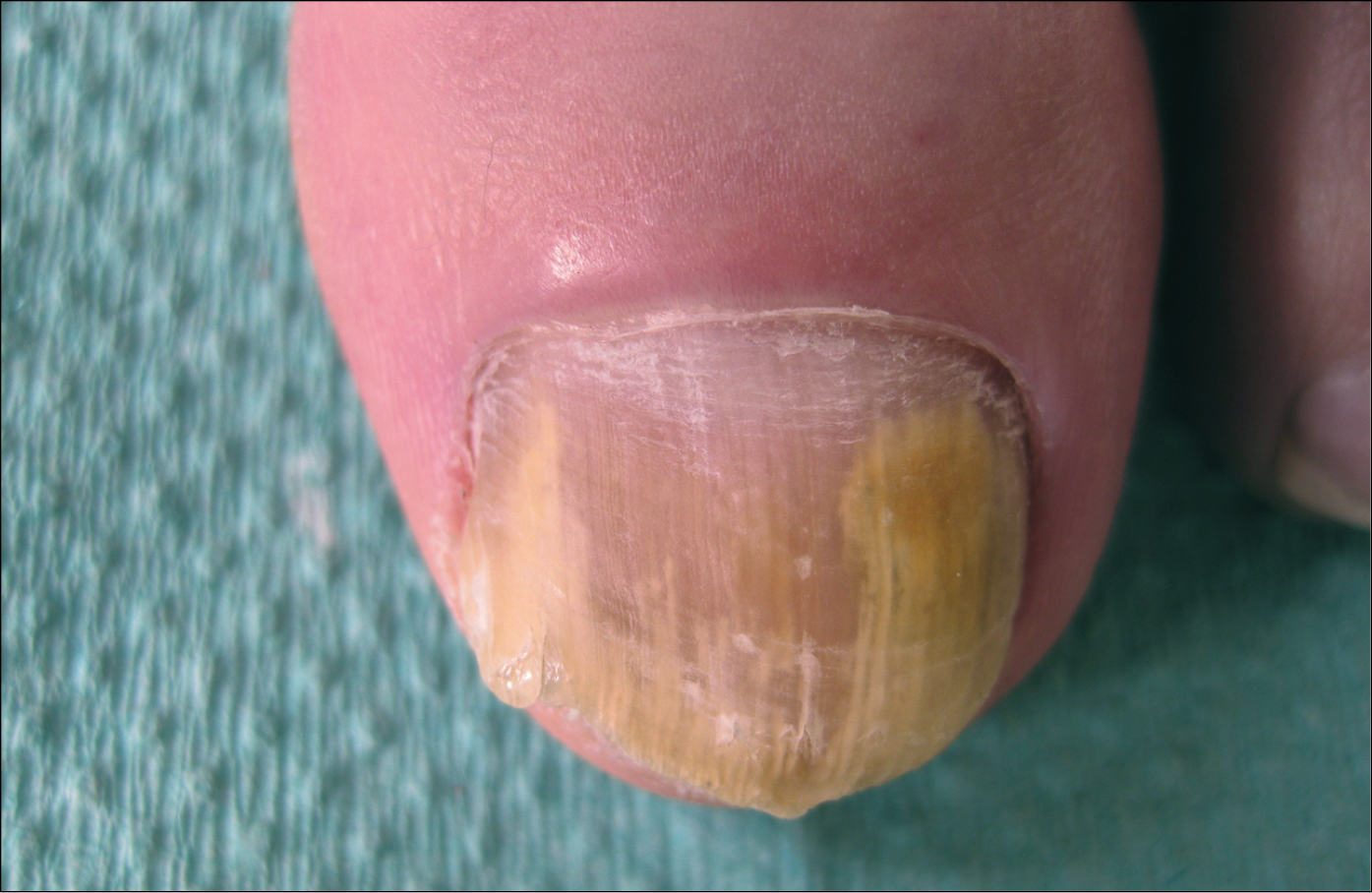
Figure 10.8-2. Distal and lateral subungual onychomycosis. The infection starts from the free edge of the nail plate and spreads towards the fold. Discolored nail plate (whitening).
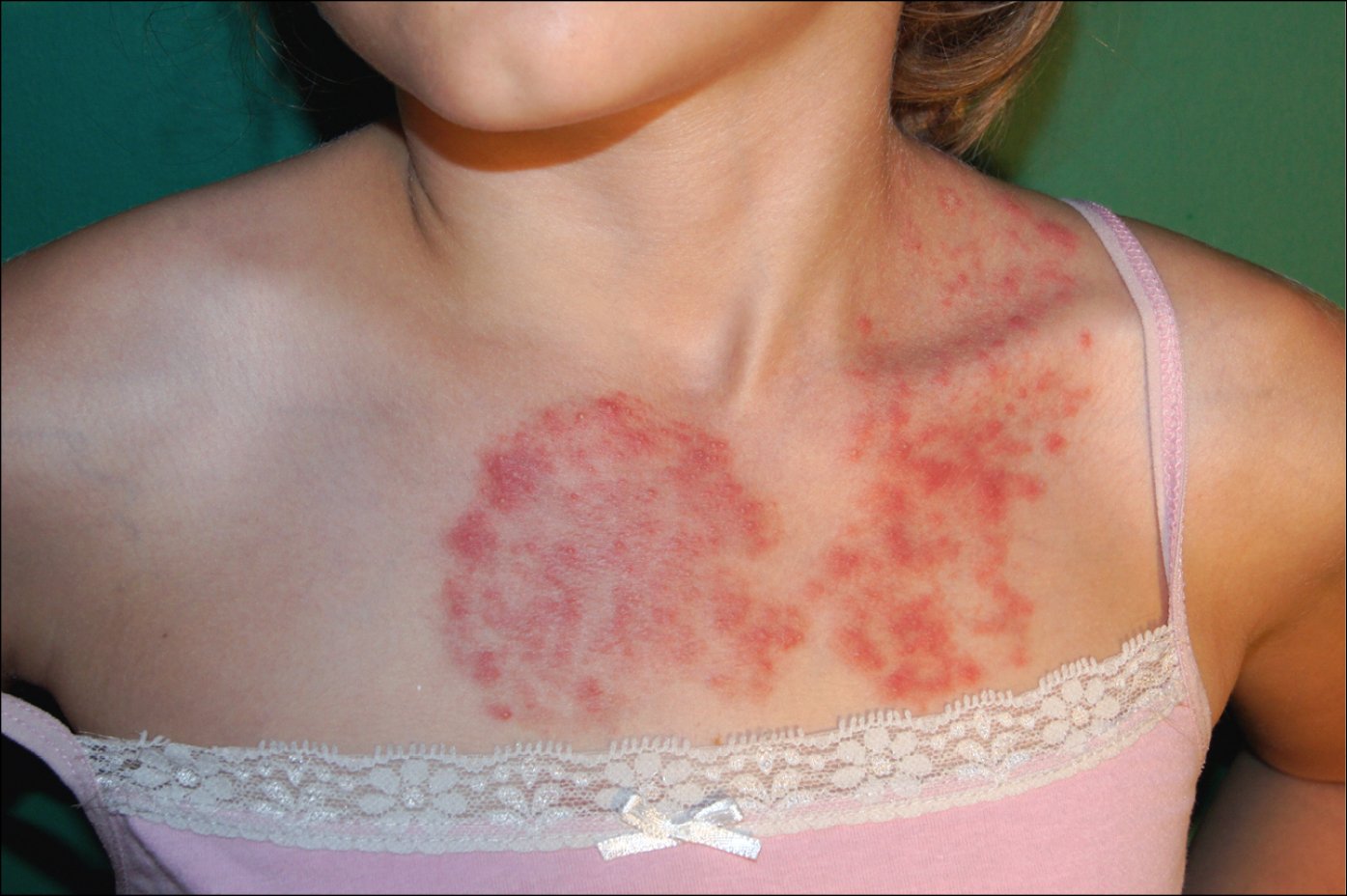
Figure 10.8-3. Tinea corporis in a child. Erythematous infiltrative skin lesion with pustules.
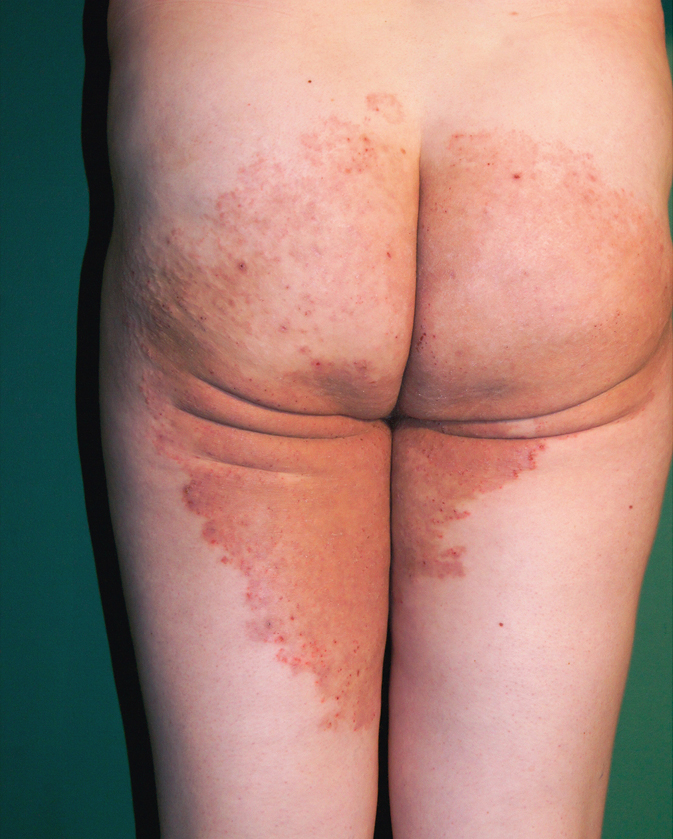
Figure 10.8-4. Tinea cruris in an adult. Lesions appear in the groins and spread peripherally. Lesions are well separated from the healthy skin, with inflammation exacerbated on the margins and less severe in the central part.
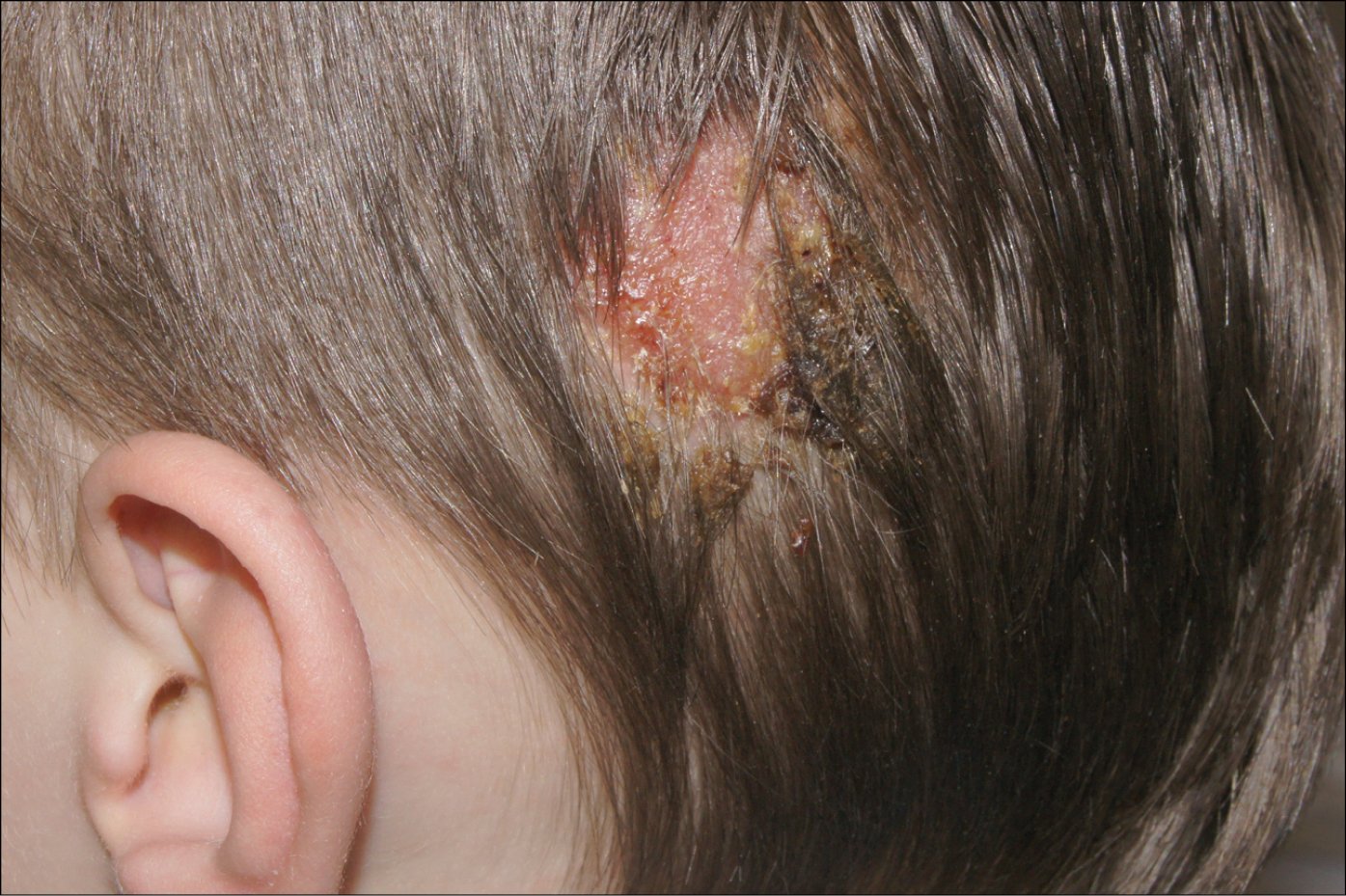
Figure 10.8-5. Tinea capitis with a significant inflammatory reaction. Inflammatory process with secretion forming a kerion celsi.