Leung AK, Barankin B, Lam JM, Leong KF, Hon KL. Tinea versicolor: an updated review. Drugs Context. 2022 Nov 14;11:2022-9-2. doi: 10.7573/dic.2022-9-2. PMID: 36452877; PMCID: PMC9677953.
Hald M, Arendrup MC, Svejgaard EL, Lindskov R, Foged EK, Saunte DM; Danish Society of Dermatology. Evidence-based Danish guidelines for the treatment of Malassezia-related skin diseases. Acta Derm Venereol. 2015 Jan;95(1):12-9. doi: 10.2340/00015555-1825. PMID: 24556907.
Gupta AK, Lane D, Paquet M. Systematic review of systemic treatments for tinea versicolor and evidence-based dosing regimen recommendations. J Cutan Med Surg. 2014 Mar-Apr;18(2):79-90. doi: 10.2310/7750.2013.13062. PMID: 24636433.
Etiology and PathogenesisTop
1. Etiologic agent: Yeast-like fungi of the genus Malassezia, most commonly Malassezia furfur, normal inhabitants of the human skin, particularly the scalp, neck, and shoulders.
2. Risk factors: Moist skin, increased sebum production, and immune system disorders. Pronounced lesions are observed in transplant recipients and persons with HIV infection.
CLINICAL FEATURES AND NATURAL HISTORYTop
Lesions are typically asymptomatic and are concentrated on the neck, shoulders, back, and chest. They may also appear on the face, particularly in children. The eruptions appear as macules of different colors, initially pink, through yellowish brown, to brown (Figure 10.8-1). In summer, following sun exposure, well-demarcated white spots are visible at the site of infection (Figure 10.8-2). The depigmentation results from inhibition of melanin production by dicarboxylic acid, a product of Malassezia. The eruptions are characterized by superficial flaking and presence of small scales. Recurrences are frequent.
Several distinct morphologic variants of tinea versicolor have been described. Inverse tinea versicolor, sometimes referred to as “tinea in versicolor,” is a variant characterized by lesions concentrated on the flexural regions, including the axilla, elbow, popliteal fossa, and groin, as well as isolated areas of the extremities.Evidence 1Low Quality of Evidence (low confidence that we know true effects of intervention). Quality of Evidence lowered due to the observational nature of data. Ferry M, Shedlofsky L, Newman A, Mengesha Y, Blumetti B. Tinea InVersicolor: A Rare Distribution of a Common Eruption. Cureus. 2020 Jan 17;12(1):e6689. doi: 10.7759/cureus.6689. PMID: 32104626; PMCID: PMC7026868. This variant has been particularly described in patients who are immunocompromised.
Atrophying tinea versicolor typically presents with numerous hypopigmented or erythematous/violaceous round to oval lesions with scaling and a depressed appearance.Evidence 2Low Quality of Evidence (low confidence that we know true effects of intervention). Quality of Evidence lowered due to observational nature of data. Haiduk J, Treudler R, Ziemer M. Atrophying tinea versicolor with epidermal atrophy. J Dtsch Dermatol Ges. 2016 Jul;14(7):740-3. doi: 10.1111/ddg.12894. Epub 2016 Feb 10. PMID: 26861589. These lesions are generally uniform in size on the same patient, ranging from a few millimeters to several centimeters, and tend to cluster. They may also have a wrinkled surface.
Follicular tinea versicolor involves the hair follicle and is characterized by asymptomatic hypo- or hyperpigmented macules localized around the follicles, typically on the chest and back.Evidence 3Low Quality of Evidence (low confidence that we know true effects of intervention). Quality of Evidence lowered due to observational nature of data. Nabatian AS, Millett CR, Heymann WR. What is your diagnosis? Folliculocentric tinea versicolor. Cutis. 2012 Sep;90(3):113, 117-8. PMID: 23094306. These macules may merge into larger patches.
Confetti-like tinea versicolor typically presents with asymptomatic, bilateral and symmetrically distributed confetti-like spots with slight scaling.Evidence 4Low Quality of Evidence (low confidence that we know true effects of intervention). Quality of Evidence lowered due to observational nature of data. Baz K, Kokturk A, Kaya TI, Ikizoglu G, Yazici AC, Bocekli E. Confetti-like pityriasis versicolor. J Eur Acad Dermatol Venereol. 2004 Mar;18(2):240-1. doi: 10.1111/j.1468-3083.2004.00871.x. PMID: 15009325.
DIAGNOSISTop
Diagnosis is commonly based on clinical assessment and confirmed by direct mycologic examination (potassium hydroxide test [10% KOH]). Cultures and skin biopsies are typically not required.
Seborrheic dermatitis, vitiligo, pityriasis rosea, pityriasis alba, secondary syphilis, progressive macular hypomelanosis.
TreatmentTop
1. Topical treatment is usually sufficient. Use antidandruff shampoos with azole derivatives (eg, ketoconazole, clotrimazole, econazole), Octopirox, ciclopirox olamine, selenium sulfide, or zinc pyrithione. The shampoo should be foamed and left on the skin for 3 to 5 minutes, then rinsed. Creams with azole derivatives are also effective. To avoid recurrences, periodic use of antifungal shampoos is indicated.
2. Use systemic treatment for severe, extensive lesions or lesions that do not respond to topical treatment. Highly effective oral antifungals include fluconazole 300 mg once weekly for 2 to 4 weeksEvidence 5Strong recommendation (benefits clearly outweigh downsides; right action for all or almost all patients). Moderate Quality of Evidence (high confidence that we know true effects of the intervention). Quality of Evidence lowered due to lack of blinding and unclear concealment. Amer MA. Fluconazole in the treatment of tinea versicolor. Egyptian Fluconazole Study Group. Int J Dermatol. 1997 Dec;36(12):940-2. doi: 10.1046/j.1365-4362.1997.00213.x. PMID: 9466206. Montero-Gei F, Robles ME, Suchil P. Fluconazole vs. itraconazole in the treatment of tinea versicolor. Int J Dermatol. 1999 Aug;38(8):601-3. doi: 10.1046/j.1365-4362.1999.00733.x. PMID: 10487450. and oral itraconazole 200 mg once daily for 5 to 7 days.Evidence 6Strong recommendation (benefits clearly outweigh downsides; right action for all or almost all patients). High Quality of Evidence (high confidence that we know true effects of the intervention). Hickman JG. A double-blind, randomized, placebo-controlled evaluation of short-term treatment with oral itraconazole in patients with tinea versicolor. J Am Acad Dermatol. 1996 May;34(5 Pt 1):785-7. doi: 10.1016/s0190-9622(96)90014-6. PMID: 8632075. Oral terbinafine and oral griseofulvin are antifungals that are not effective for the treatment of tinea versicolor.
preventionTop
Specific prevention regimens include topical application of azoles on previously affected sites daily, 2 weeks before expected sun exposure; antifungal shampoo application twice weekly; and oral itraconazole 200 mg twice daily, one day per month for 6 months.
Good personal hygiene.
FiguresTop
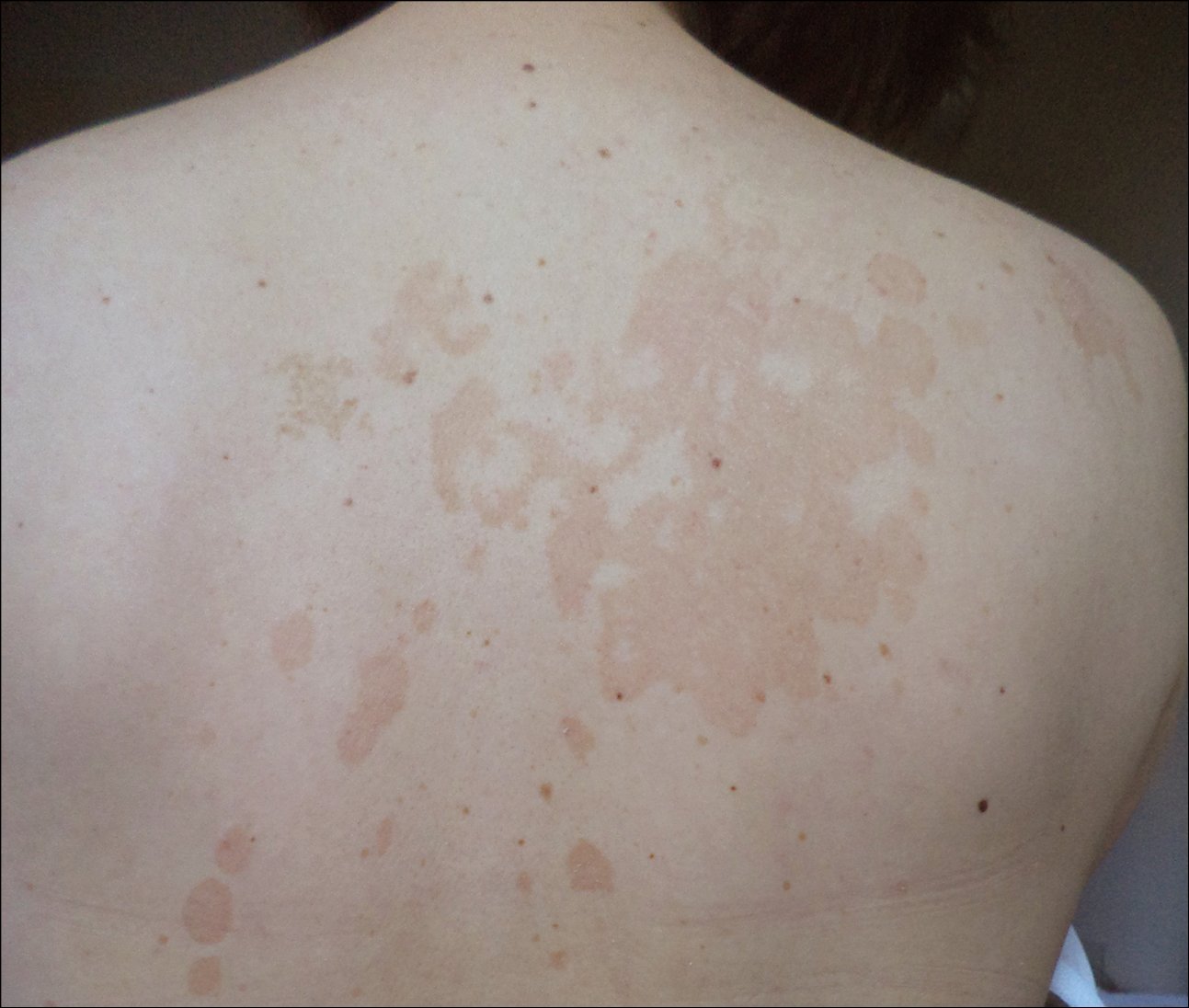
Figure 10.8-1.
Tinea versicolor. Numerous yellowish-brown macules on the trunk.
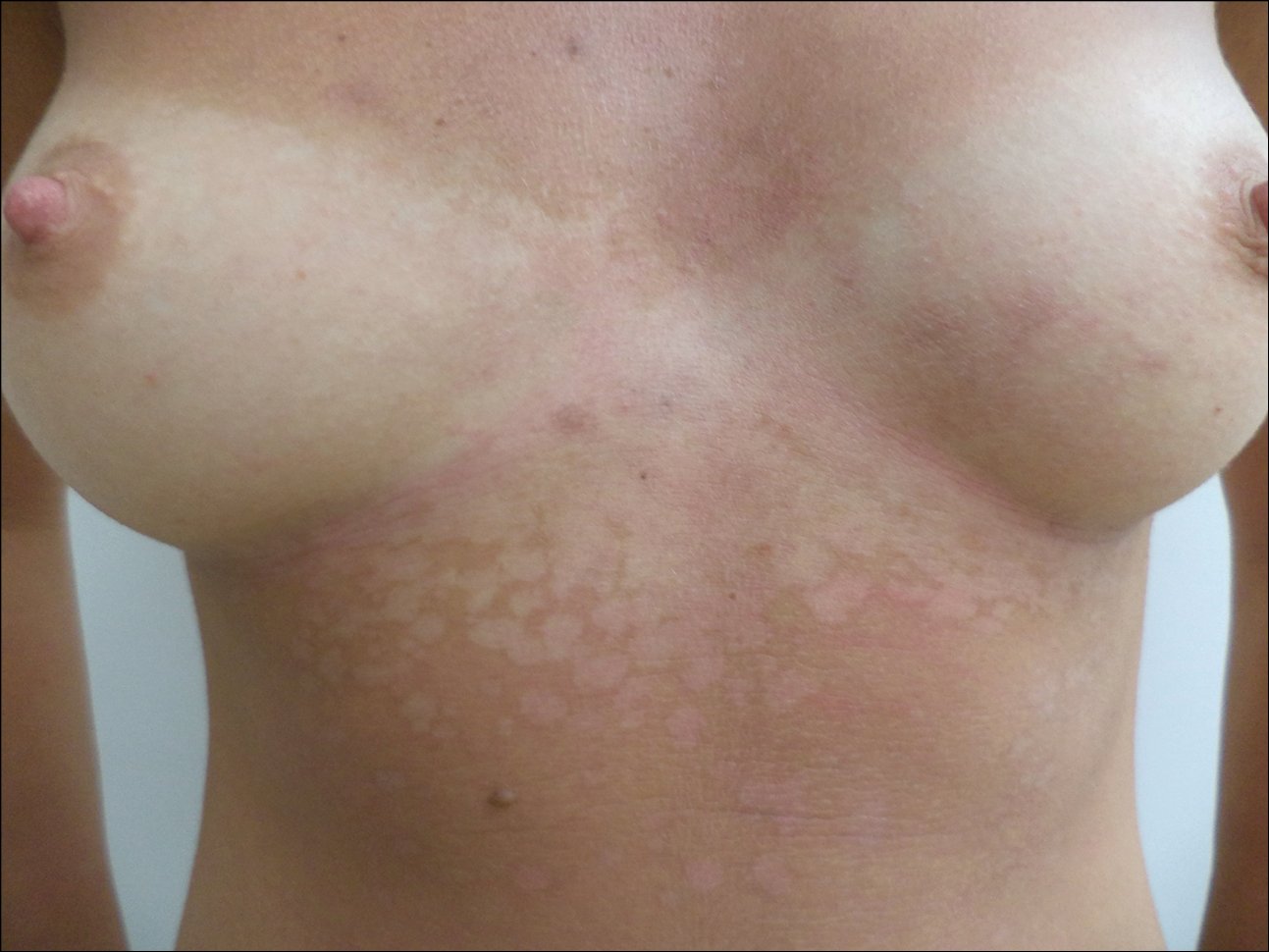
Figure 10.8-2.
Tinea versicolor. Numerous depigmented macules on the trunk, visible in summer following sun exposure.