Definition, Etiology, PathogenesisTop
Fixed drug eruption (FDE) is a distinctive skin reaction characterized by development of ≥1 round or oval erythematous patch, which characteristically recurs at the same sites as a result of systemic exposure to the same drug. The lesions eventually resolve with postinflammatory hyperpigmentation. Readministration of the offending drug affects prior sites and occasionally may cause new lesions to develop. Sometimes repeated exposure to the causative drug may not cause reignition of the previous lesions, perhaps due to a refractory period.
FDE occurs in 1% to 3% of patients taking drugs. The incidence of FDE ranges from 2.5% to 22% of all cutaneous adverse drug reactions. FDEs tend to occur in patients aged 20 to 40 years although they have been reported in all age groups.
Only 1 drug is typically involved; however, cross-sensitivity to related drugs may sometimes occur. Rarely separate drugs may cause independent FDEs. FDE may be caused by any route of ingestion, such as oral, rectal, or intravenous.
Causative agents include:
1) Acetaminophen (INN paracetamol).
2) Tetracycline antibiotics (doxycycline, minocycline).
3) Other antibiotics (amoxicillin, metronidazole, erythromycin).
4) Sulfonamides (trimethoprim with sulfamethoxazole [most common] and sulfasalazine).
5) Acetylsalicylic acid (ASA).
6) Nonsteroidal anti-inflammatory drugs (NSAIDs), including ibuprofen, diclofenac, and naproxen.
7) Sedatives (barbiturates, benzodiazepines, and chlordiazepoxide).
8) Dapsone.
9) Anticonvulsants, such as phenytoin and phenobarbital.
10) Sildenafil, tadalafil.
11) Other agents such as pseudoephedrine and methylphenidate.
The pathogenesis of FDE is unclear although a cell-mediated cytotoxic mechanism is suggested. It is thought that the offending drug acts as a hapten that binds to basal keratinocytes. This activates cytotoxic T cells in the epidermis to release cytokines such as interferon gamma, tumor necrosis factor (TNF)-alpha, granzyme B, and perforin. The keratinocytes upregulate intercellular adhesion molecule-1 (ICAM1) expression, which aids the infiltration of helper T cells to the affected site. The CD8 cells and cytokines destroy local skin cells. Changes in cell surface markers also allow CD4 infiltration into active lesions. CD4 cells produce interleukin 10 and suppress immune function, causing a resting lesion. As the inflammatory response resolves, CD8+ effector memory T cells persist in the epidermis to release more cytokines upon re-exposure to the causative drug.
Clinical Features and Natural HistoryTop
FDE presents as well-defined, round or oval dusky erythematous or violaceous macules or patches (Figure 4.3-1). Commonly affected sites include the face, especially lips, and genitalia, but other sites can also be involved, including the extremities, hands and feet, trunk, buttocks, and perianal areas. FDE usually develops within 30 minutes to 8 hours of exposure to the drug, but it may take ≤2 weeks to develop. The lesions usually persist for days to weeks before resolving spontaneously. As the FDE starts to heal, the lesions form crusts and scale before fading to a purple or dusky brown color. These hyperpigmented patches often persist for a while and resolve over time if the causative drug is avoided. Hyperpigmentation tends to be more pronounced in those with a darker skin color.
FDE often has no accompanying symptoms. If present, symptoms are often mild and include pruritus, burning, or stinging sensation. Systemic symptoms such as fever, malaise, nausea, and anorexia are rare but may occur in generalized bullous variants.
Upon re-exposure to the same drug, lesions appear at the same exact location and new lesions may appear on other areas not previously involved.
Several variants of FDE have been reported, including:
1) Pigmented FDE.
2) Generalized FDE.
3) Linear FDE.
4) Wandering (migrating) FDE.
5) Nonpigmenting FDE, typically described with pseudoephedrine, piroxicam, cotrimoxazole, sorafenib, and tadalafil.
6) Bullous FDE (localized or generalized).
7) Eczematous FDE.
8) Psoriasiform FDE.
9) Urticarial FDE.
10) Erythema dyschromicum perstans–like FDE.
DiagnosisTop
Diagnosis is typically based on clinical history. Patients should be asked about recent medications, prior episodes of skin lesions at the same involved sites, or other past adverse drug reactions. Occasionally patients may not realize that they have a drug-related lesion and may be convinced that it is due to an insect bite.
Physical examination shows a well-defined, round or oval erythematous patch, which gradually fades with residual hyperpigmentation. The center of the patch may blister or become necrotic over several days. With re-exposure to the drug, resting hyperpigmented macules reactivate. Certain medications tend to follow site-specific patterns. For example, trimethoprim/sulfamethoxazole, sulfonamides, and tetracyclines tend to affect the genital region, and naproxen, the lips.
1. Patch testing (topical provocation): Should be performed at the site of the previous FDE lesion. Doing the test at a noninvolved area may yield a false-negative result. An open test is recommended, with the drug being compounded in white petrolatum at a concentration of 1% to 10%. A positive test result is indicated by erythema that starts within 24 hours and lasts ≥6 hours. If the test result is negative, a higher concentration of drugs or a different vehicle (eg, ethanol or dimethyl sulfoxide) may be used. The test may be repeated every 12 hours, for a maximum of 4 times.
2. Oral provocation: The gold standard in diagnosing FDE, typically follows patch testing. A delay between patch testing and oral provocation is recommended due to a refractory period in FDE. Oral provocation is performed using a subtherapeutic initial dose, and a positive test result is indicated by a reactivation of an old FDE site within 10 to 30 minutes; however, a delay of ≤18 hours is possible. If the test result is negative, the dose of the drug is increased every 12 to 24 hours until reaching a full dose. Oral provocation is started with the least likely drugs and negative patch test agents first, followed by more likely causative drugs. The test should be performed by an experienced allergy or dermatology specialist. Oral and systemic provocation is contraindicated in generalized FDE and in children.
3. Skin biopsy: May be performed if diagnosis is unclear. Histology shows interface dermatitis, with vacuolar change and Civatte bodies. Other prominent features may include dyskeratosis and individual necrotic keratinocytes within the epidermis. Spongiosis, dermal edema, eosinophils, and occasional neutrophils may also be present. In older inactive lesions histology may show pigmentary incontinence, mild acanthosis, hyperkeratosis, or relatively few inflammatory cells.
TreatmentTop
The mainstay of treatment for FDE is to identify the offending agent, discontinue its use, and avoid it in the future. Patients should be counseled about medication avoidance and possible cross-reactions and advised to notify their physicians about any FDE or previous adverse drug reactions.
Medical treatment is generally not needed. Oral H1 antihistamines (eg, cetirizine, hydroxyzine) and topical glucocorticoids (eg, 0.05% betamethasone dipropionate) can be used for symptomatic treatment if symptoms such as itching or stinging are present. Topical glucocorticoids may also reduce the rates of hyperpigmentation following resolution of FDE. For erosive cases, wet compresses may be used and followed by the application of hydrated petrolatum or petrolatum gauze. If superimposed bacterial infection is suspected, topical (2% fusidic acid) or oral antibiotics may be used.
FiguresTop
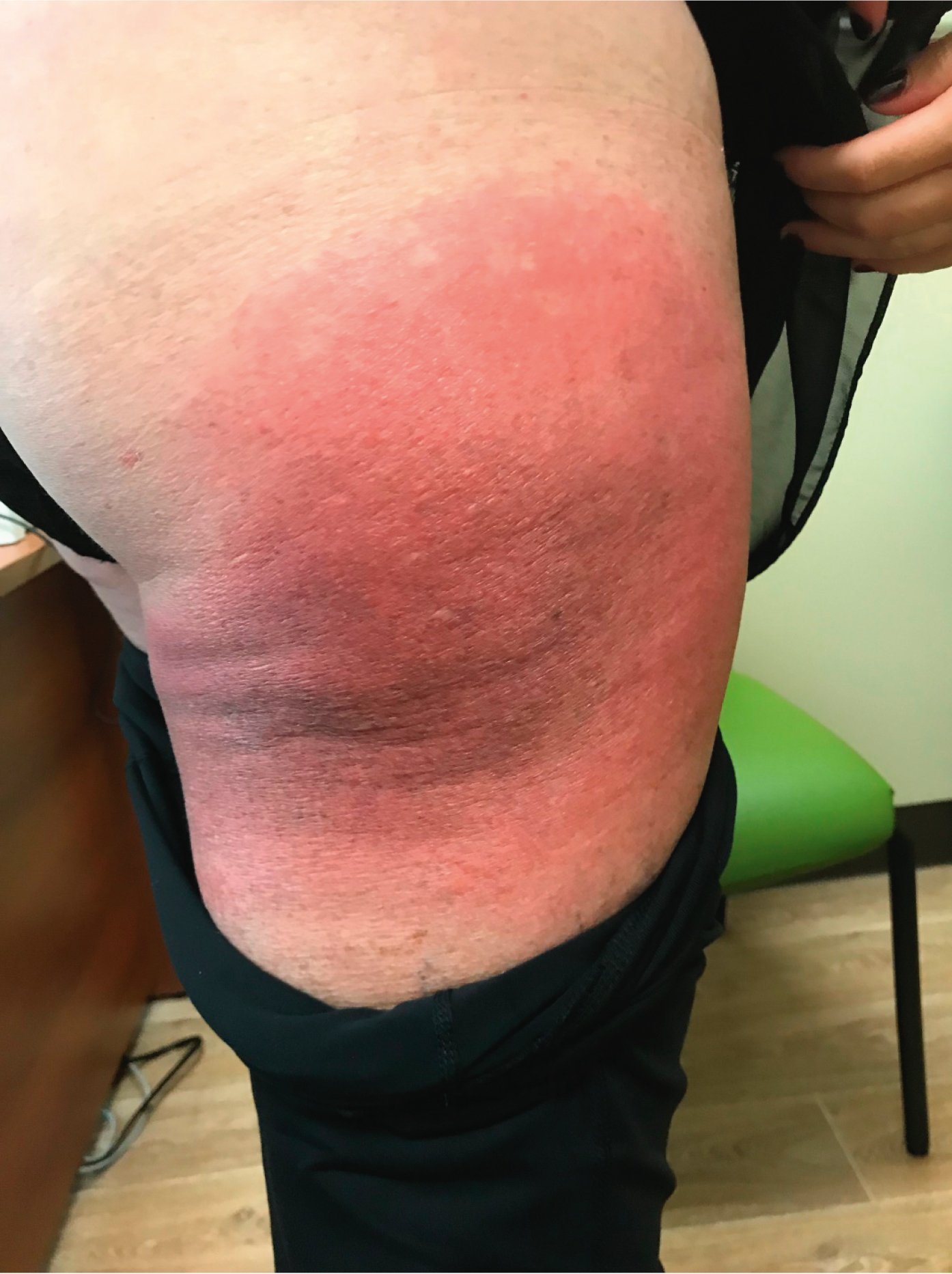
Figure 4.3-1. Well-defined erythematous patch with a dusky red center occurring for the third time on the same exact site on the right thigh upon exposure to amoxicillin. Photograph courtesy of Dr Mohannad Abu-Hilal.