Vahanian A, Beyersdorf F, Praz F, et al; ESC/EACTS Scientific Document Group. 2021 ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2022 Feb 12;43(7):561-632. doi: 10.1093/eurheartj/ehab395. Erratum in: Eur Heart J. 2022 Feb 18;: PMID: 34453165.
Otto CM, Nishimura RA, Bonow RO, et al. 2020 ACC/AHA Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2021 Feb 2;143(5):e35-e71. doi: 10.1161/CIR.0000000000000932. Epub 2020 Dec 17. Erratum in: Circulation. 2021 Feb 2;143(5):e228. Erratum in: Circulation. 2021 Mar 9;143(10):e784. PMID: 33332149.
Definition, Etiology, Pathogenesis Top
Mitral regurgitation (MR) is a backward blood flow from the left ventricle (LV) to the left atrium (LA) due to an incomplete closure of the mitral valve leaflets. In 10% to 40% of people in whom Doppler echocardiography is performed results show a mild regurgitant jet with no evident abnormalities of the valve apparatus (so-called physiologic regurgitation).
Primary (organic) MR is due to primary damage of the valve apparatus (leaflets, chordae tendineae, papillary muscles, or a combination of these). Secondary (functional) MR is due to changes in LV/LA size and function (eg, in ischemic or dilated cardiomyopathy) in the presence of structurally normal valve apparatus.
Etiology of chronic MR:
1) Primary: Degenerative lesions (myxomatous mitral valve disease [variable extent with bileaflet involvement known as the “Barlow valve”], idiopathic rupture of the chordae tendineae [fibroelastic deficiency]), systemic connective tissue disorders (Marfan syndrome, Ehlers-Danlos syndrome), calcification of the mitral annulus, infective endocarditis (infectious or noninfectious—eg, associated with antiphospholipid syndrome), rheumatic disease, drug mediated (ergotamines, appetite suppressants [eg, fenfluramine; currently withdrawn]), radiation mediated, congenital (eg, mitral valve clefts).
2) Secondary: Diseases of the myocardium (ischemic heart disease, nonischemic dilated cardiomyopathy, storage and infiltrative diseases [amyloidosis, eosinophilic cardiomyopathy, carcinoid syndrome, endomyocardial fibrosis]), left atrial enlargement (“atriogenic” MR).
Etiology of acute MR:
1) Primary (organic): Lesions of the valve leaflets (infective endocarditis, leaflet trauma, eg, after balloon valvotomy), rupture of the chordae tendineae (idiopathic, myxomatous degeneration, infective endocarditis, acute rheumatic fever, leaflet trauma), papillary muscle rupture (most commonly following inferior ST-segment elevation myocardial infarction [STEMI]).
2) Secondary (functional): Acute leaflet restriction with or without reduction in closing forces (acute myocardial infarction [MI], acute LV dilation [eg, acute myocarditis]).
Clinical Features and Natural History Top
1. Symptoms: Mild or moderate chronic MR is usually asymptomatic (in the case of slow progression of regurgitation—even if it is severe—the symptoms may be minor). With time, patients develop symptoms related to changes in LV function and filling pressure, left atrial compliance, pulmonary artery pressure, and right ventricular function, with increased risk of arrhythmias (most commonly atrial fibrillation [AF] and less commonly ventricular arrhythmias). In acute MR, sudden dyspnea and hypotension or cardiogenic shock may occur. Classification of severity: Table 1.
2. Signs: A holosystolic murmur, whose loudness is usually correlated with the size of the regurgitant volume (except for ischemic regurgitation); a possible short diastolic rumble (in severe MR); duration can be variable with late systolic murmur preceded by a systolic click associated with mitral valve prolapse; a diminished first heart sound (in clinically significant MR); splitting of the second heart sound; third heart sound (correlating with the regurgitant volume and with LV enlargement); laterally displaced apex. Pulmonary crepitations may occur. In patients with severe MR and pulmonary hypertension, symptoms of right ventricular failure (see Chronic Heart Failure) may be present.
3. Natural history: In functional MR, disease progression is related to the underlying condition (LV disease). Acute MR is rapidly progressive and usually fatal when left without surgical treatment: 25% of patients with moderate or severe MR related to acute MI die within 30 days, and 50% die within one year. In the case of papillary muscle rupture in the course of acute MI, 95% of patients die within two weeks. Chronic MR may remain asymptomatic for over a decade. The regurgitant volume is of a significant prognostic value in asymptomatic patients. Uncorrected severe MR may lead to irreversible asymptomatic LV dysfunction.
Diagnosis Top
Diagnosis is based on clinical features (if present) and echocardiography.
1. Electrocardiography (ECG) is usually normal; the most frequent abnormalities include AF and atrial flutter. Patients with preserved sinus rhythm may have features of left atrial enlargement (or enlargement of both atria in patients with coexisting tricuspid regurgitation). Signs of LV hypertrophy and pulmonary hypertension may be present in chronic severe MR.
2. Chest radiography: Significant LV and left atrial enlargement; right ventricular and right atrial enlargement in patients with coexisting tricuspid regurgitation and pulmonary hypertension. Patients with acute MR have features of pulmonary congestion with a normal cardiac silhouette. Calcifications of the mitral annulus may be present.
3. Echocardiography (Figure 1) is the primary diagnostic modality used to detect and classify the severity of regurgitation, define the mechanism of regurgitation, detect secondary structural changes (effects on LV and LA), and estimate pulmonary artery pressures. In the case of equivocal results of transthoracic imaging, transesophageal echocardiography is often helpful.
4. Exercise stress testing is helpful for objective evaluation of exercise tolerance. Echocardiographic stress test can be used for noninvasive assessment of exertional increase in pulmonary artery systolic pressures and potential dynamic regurgitation severity changes.
5. Cardiac catheterization and coronary angiography are rarely performed in MR, except to assess for concomitant coronary artery disease in patients referred for mitral valve surgery in whom coronary disease is a clinical concern (>40 years of age, coronary disease risk factors).
6. Magnetic resonance imaging (MRI) can further define MR severity if the echocardiographic image is equivocal. It can also serve as a more reliable determination of LV volumes and ejection fraction, and potentially add prognostic information (late gadolinium enhancement of the myocardium).
On physical examination, differential diagnosis includes other valvular lesions that result in systolic murmurs (eg, aortic stenosis and tricuspid regurgitation). Echocardiography usually readily differentiates these lesions or diagnoses multiple lesions if concurrently present.
Treatment Top
Treatment of Acute Mitral Regurgitation
1. Vasodilators (nitroglycerin or sodium nitroprusside). In the case of shock, these are used in combination with intra-aortic balloon counterpulsation (the latter is contraindicated in patients with coexisting significant aortic regurgitation) and inotropes as indicated. Agents and dosage: see Table 3 in Essential Hypertension.
2. Surgical treatment is necessary in all patients with severe acute MR who are surgical candidates; emergency surgery is necessary in the case of hemodynamic instability. Depending on the anatomy, this includes either mitral valvuloplasty (eg, partial leaflet resection, annuloplasty using a prosthetic ring) or mitral valve replacement (bioprosthetic or mechanical). Transcatheter mitral valve intervention options have been used for patients with high/prohibitive surgical risk.
Treatment of Chronic Mitral Regurgitation
Management of severe chronic primary MR: In general, medical therapy, structural interventions (surgical or transcatheter), or both may be used, depending mainly on the presence of symptoms, LV function and size, and need for coronary revascularization:
1) Primary MR: Mitral valve repair is preferred to replacement (when effective and durable repair can be completed). Class 1 indications for surgical intervention are left ventricular ejection fraction (LVEF) ≤60%, significant LV dilation (LV end-systolic diameter ≥40 mm), and onset of symptoms. Earlier surgical intervention can be considered in the absence of these thresholds, weighing the interventional risk, probability of repair, and presence of prognostic factors (with lower threshold for intervention in lower-risk patients and those with a high probability of repair). Prognostic findings that indicate worse outcomes in the setting of severe MR include LA dilatation (LA volume index [LAVI] ≥60 mL/m2), presence of AF, pulmonary artery systolic pressure (PASP) >50 mm Hg, and progressive LV dilatation and reductions in LVEF on serial echocardiograms.
In patients with very poor LV function (LVEF <30%), surgery can be considered in experienced hands. Percutaneous mitral valve repair (eg, edge-to-edge repair) is an alternative in patients with high/prohibitive surgical risk. Medical therapy has a limited role for treatment of complications including heart failure and atrial fibrillation. Afterload reduction is recommended for treatment of hypertension when present and not recommended as a strategy to alter the natural history of the pathology.
2) Secondary MR: Patients with severe secondary MR should receive optimal guideline-directed medical therapy based on LVEF, including angiotensin-converting enzyme inhibitors (ACEIs), angiotensin receptor blockers (ARBs), or angiotensin receptor-neprilysin inhibitors (ARNIs), beta-blockers, aldosterone antagonists, sodium-glucose cotransporter-2 (SGLT-2) inhibitors, ivabradine, and diuretics as needed. Cardiac resynchronization can reduce MR in those qualifying based on LVEF and QRS duration.Evidence 1Strong recommendation (benefits clearly outweigh downsides; right action for all or almost all patients). Moderate Quality of Evidence (moderate confidence that we know true effects of the intervention). Quality of Evidence lowered due to lack of blinding in one trial and a short follow-up time. Cleland JG, Daubert JC, Erdmann E, et al; Cardiac Resynchronization-Heart Failure (CARE-HF) Study Investigators. The effect of cardiac resynchronization on morbidity and mortality in heart failure. N Engl J Med. 2005 Apr 14;352(15):1539-49. Epub 2005 Mar 7. PubMed PMID: 15753115. Abraham WT, Fisher WG, Smith AL, et al; MIRACLE Study Group. Multicenter InSync Randomized Clinical Evaluation. Cardiac resynchronization in chronic heart failure. N Engl J Med. 2002 Jun 13;346(24):1845-53. PubMed PMID: 12063368. Strategies to optimize AF (rhythm control) may improve the severity of MR with a probable mechanism of atriogenic MR. Patients with persistent symptomatic severe MR despite therapy for LV dysfunction should be referred to an interdisciplinary heart team to consider percutaneous or surgical intervention. When surgery is performed, mitral valve replacement rather than surgical repair is associated with less recurrent MR.Evidence 2Weak recommendation (benefits likely outweigh downsides, but the balance is close or uncertain; an alternative course of action may be better for some patients). Moderate Quality of Evidence (moderate confidence that we know true effects of intervention). Quality of Evidence lowered due to imprecision in the critical outcome of mortality. Goldstein D, Moskowitz AJ, Gelijns AC, et al; CTSN. Two-Year Outcomes of Surgical Treatment of Severe Ischemic Mitral Regurgitation. N Engl J Med. 2016 Jan 28;374(4):344-53. doi: 10.1056/NEJMoa1512913. Epub 2015 Nov 9. PubMed PMID: 26550689. Surgery is not routinely indicated in patients with moderate MR who undergo CABG.Evidence 3Weak recommendation (downsides likely outweigh benefits, but the balance is close or uncertain; an alternative course of action may be better for some patients). Moderate Quality of Evidence (moderate confidence that we know true effects of intervention). Quality of Evidence lowered due to the relatively short follow-up (indirectness). Smith PK, Puskas JD, Ascheim DD, et al; Cardiothoracic Surgical Trials Network Investigators. Surgical treatment of moderate ischemic mitral regurgitation. N Engl J Med. 2014 Dec 4;371(23):2178-88. doi: 10.1056/NEJMoa1410490. Epub 2014 Nov 18. PubMed PMID: 25405390; PubMed Central PMCID: PMC4303577.Chan KM, Punjabi PP, Flather M, et al; RIME Investigators. Coronary artery bypass surgery with or without mitral valve annuloplasty in moderate functional ischemic mitral regurgitation: final results of the Randomized Ischemic Mitral Evaluation (RIME) trial. Circulation. 2012 Nov 20;126(21):2502-10. doi: 10.1161/CIRCULATIONAHA.112.143818. Epub 2012 Nov 7. PubMed PMID: 23136163. For patients without other indications for sternotomy and with an appropriate anatomy, percutaneous mitral valve repair with mitral valve clip(s) in experienced centers should be considered in appropriately selected, medically optimized patients to reduce the rates of heart failure admissions and mortality.Evidence 4Weak recommendation (benefits likely outweigh downsides, but the balance is close or uncertain; an alternative course of action may be better for some patients). Moderate Quality of Evidence (moderate confidence that we know true effects of intervention). Quality of Evidence lowered due to the short period of follow-up (indirectness). Stone GW, Lindenfeld J, Abraham WT, et al; COAPT Investigators. Transcatheter Mitral-Valve Repair in Patients with Heart Failure. N Engl J Med. 2018 Dec 13;379(24):2307-2318. doi: 10.1056/NEJMoa1806640. Epub 2018 Sep 23. PubMed PMID: 30280640. Obadia JF, Messika-Zeitoun D, Leurent G, et al; MITRA-FR Investigators. Percutaneous Repair or Medical Treatment for Secondary Mitral Regurgitation. N Engl J Med. 2018 Dec 13;379(24):2297-2306. doi: 10.1056/NEJMoa1805374. Epub 2018 Aug 27. PubMed PMID: 30145927. Glower DD, Kar S, Trento A, et al. Percutaneous mitral valve repair for mitral regurgitation in high-risk patients: results of the EVEREST II study. J Am Coll Cardiol. 2014 Jul 15;64(2):172-81. doi: 10.1016/j.jacc.2013.12.062. PubMed PMID: 25011722.Feldman T, Foster E, Glower DD, et al; EVEREST II Investigators. Percutaneous repair or surgery for mitral regurgitation. N Engl J Med. 2011 Apr 14;364(15):1395-406. doi: 10.1056/NEJMoa1009355. Epub 2011 Apr 4. Erratum in: N Engl J Med. 2011 Jul 14;365(2):189. Glower, Donald G [corrected to Glower, Donald D]. PubMed PMID: 21463154.
Vasodilators (carvedilol, isosorbide mononitrate, ACEIs, angiotensin-receptor blockers): These are most effective in patients with contraindications to surgery who have LV enlargement, significant systolic LV dysfunction, and severe symptoms.Evidence 5Weak recommendation (benefits likely outweigh downsides, but the balance is close or uncertain; an alternative course of action may be better for some patients). Low Quality of Evidence (low confidence that we know true effects of the intervention). Quality of Evidence lowered due to the small number of patients, indirect outcomes, and short follow-up. Ahmed MI, Aban I, Lloyd SG, et al. A randomized controlled phase IIb trial of beta(1)-receptor blockade for chronic degenerative mitral regurgitation. J Am Coll Cardiol. 2012 Aug 28;60(9):833-8. doi: 10.1016/j.jacc.2012.04.029. Epub 2012 Jul 18. PubMed PMID: 22818065; PubMed Central PMCID: PMC3914413. Levine AB, Muller C, Levine TB. Effects of high-dose lisinopril-isosorbide dinitrate on severe mitral regurgitation and heart failure remodeling. Am J Cardiol. 1998 Nov 15;82(10):1299-301, A10. PubMed PMID: 9832115. In asymptomatic patients with minor LV enlargement, vasodilators offer little or no benefit. Agents and dosage: see Table 5 in Essential Hypertension.
Follow-Up Top
Follow-up: Table 2.
Complications Top
AF, heart failure and pulmonary edema, pulmonary hypertension, sudden cardiac death (in patients with a flail leaflet).
Prognosis Top
The annual mortality rate in severe chronic structural MR without surgical treatment is 5%.
Tables and FiguresTop
|
Regurgitation | |||
|
Mild |
Moderate |
Severe | |
|
Effective regurgitant orifice area (cm2) |
<0.20 |
0.2-0.39 |
≥0.40 |
|
Regurgitant volume (mL) |
<30 |
30-59 |
≥60 |
|
Regurgitant fraction (%) |
<30 |
30-49 |
≥50 |
|
PASP (mm Hg) |
<30 |
30-50 |
>50 |
|
Based on Circulation 2021;143(5): e72-e227. | |||
|
MVA, mitral valve area; MVG, mitral valve gradient; PASP, pulmonary artery systolic pressure. | |||
|
Severity of regurgitation |
Follow-up |
|
Mild |
Every 5 years |
|
Moderate |
Every 1-2 years |
|
Severe |
Every year |
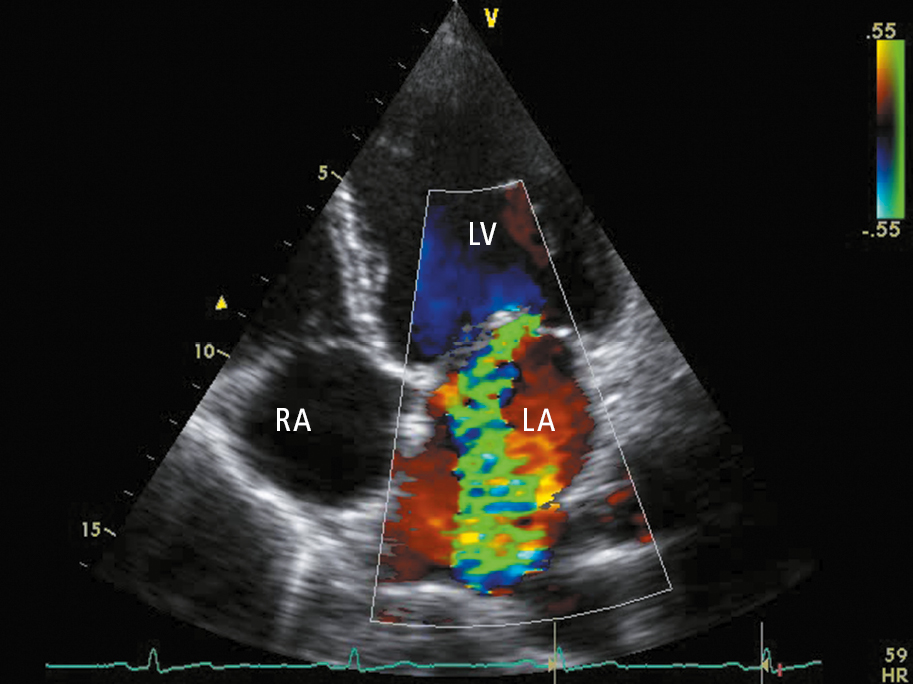
Figure 3.18-4. Transthoracic echocardiography (TTE) (apical 4-chamber view): mitral regurgitation (regurgitation jet marked in green). LA, left atrium; LV, left ventricle; RA, right atrium.