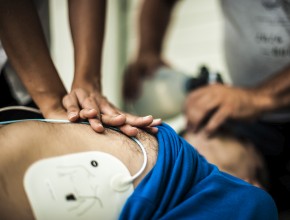
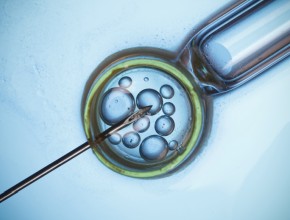
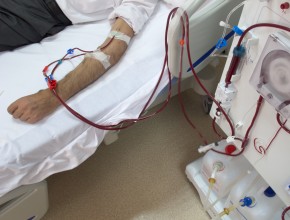
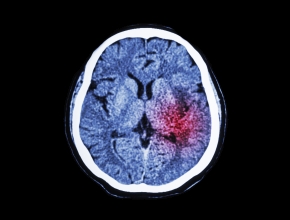
The role of pharmacists in deprescribing medication
This study examined the influence of pharmacists based in Quebec, Canada, in reevaluating the use of and possibly stopping medications from one of 4 drug classes that have the potential to adversely affect elderly patients and likely have safer alternatives: sedative-hypnotics, sedating antihistamines, glyburide, and nonsteroidal anti-inflammatory drugs (NSAIDs).
In the intervention group, the pharmacists sent educational brochures to >200 patients (≥65 years of age, taking ≥1 of the above-mentioned drugs) and at the same time provided each participant’s physician with evidence-based pharmaceutical opinions exploring the possibility of deprescribing.
After 6 months, discontinuation of sedative-hypnotic drugs occurred in 43% of patients in the intervention group versus 9% in the control group; discontinuation of glyburide, in 31% versus 14%; and discontinuation of NSAIDs, in 58% versus 22%. Among patients tapering the doses of sedative-hypnotic drugs, 38% reported withdrawal symptoms. All between-group differences were statistically significant.
When dispensing medications ordered by qualified practitioners, should pharmacists advise patients about the potential need/possibility/benefit of stopping the drugs? Click here to submit your answer via MetaClinician and see what your peers would do.
COPD: No clear benefits of adding theophylline to treatment
Criner GJ, Celli BR. Failure of Low-Dose Theophylline to Prevent Exacerbations in Patients With COPD. JAMA. 2018 Oct 16;320(15):1541-1542. doi: 10.1001/jama.2018.14295. PubMed PMID: 30326108.
Theophylline continues to be part of treatment in patients with chronic obstructive pulmonary disease (COPD).
This study included >1500 patients with a ratio of forced expiratory volume in the first second (FEV1) to forced vital capacity (FVC) of <0.7, a smoking history of >10 pack-years, and ≥2 exacerbations treated with antibiotics, oral corticosteroids, or both in the previous year. At baseline, all patients were treated with inhaled corticosteroids (ICS): around 2% received ICS alone, around 2% received a combination of ICS and long-acting muscarinic antagonists (LAMA), around 17% were using a combination of ICS and long-acting beta2-agonists (LABA), and the rest (close to 80%) were on triple inhaled therapy (ICS/LABA/LAMA). Patients were randomized to receive either low-dose theophylline (200 mg once or twice a day to achieve plasma concentrations of 1-5 mg/L) or placebo.
Over the course of a 1-year observation period, the mean number of moderate to severe exacerbations requiring treatment with antibiotics, oral corticosteroids, or both was the same (2.24 exacerbations/year in the theophylline group vs 2.23 exacerbations/year in the placebo group). Serious adverse effects also occurred with similar frequency (13.2% vs 14.0%, respectively). There were fewer COPD hospital admissions in the theophylline group: 0.17 versus 0.24 per patient per year (mean difference, −0.07; 95% CI, −0.13 to −0.01).
The authors interpret the results as not supporting the use of low-dose theophylline in patients at risk of COPD exacerbations. In the accompanying editorial, the authors point out the slightly decreased COPD hospitalization rate among patients treated with theophylline, noting that this potential beneficial effect was observed among those with a history of previous hospitalizations. The authors conclude this leaves the door open for further studies in this particular population.
Do you use theophylline when trying to prevent COPD exacerbations among patients at risk? Click here to submit your answer via MetaClinician and see what your peers would do.
PCSK9 in patients with ACS
Use of proprotein convertase subtilisin/kexin type 9 (PCKS9) inhibitors improves the prognosis in patients with acute coronary syndrome (ACS) whose cholesterol levels are not controlled by statins.
The risk of a recurrent acute atherosclerotic event after an acute coronary event decreases among those treated with cholesterol-lowering drugs (in most previous studies, statins).
Almost 19,000 patients who had had an ACS within the previous 12 months and had low-density lipoprotein (LDL) cholesterol levels ≥1.8 mmol/L (70 mg/dL) while receiving high-dose statin therapy were treated with alirocumab, a human monoclonal antibody to PCSK9. The target cholesterol level in the active group was from 25 through 50 mg/dL (0.6-1.3 mmol/L).
After a median duration of treatment of 2.8 years, patients treated with alirocumab were less likely to die (3.5% vs 4.1%; hazard ratio [HR], 0.85; 95% CI, 0.73-0.98) and less likely to have a composite end point of death from coronary heart disease, nonfatal myocardial infarction, fatal or nonfatal ischemic stroke, or unstable angina requiring hospitalization (9.5% vs 11.1%; HR, 0.85; 95% CI, 0.78-0.93).
McMaster editors’ commentary: At the rates observed in this study, one needs to treat >160 patients for 2.8 years to avoid 1 death and >60 patients to avoid 1 composite outcome. The estimated price of using this medication in 60 patients in some jurisdictions may be as high as exceeding US $2 million; it will be likely lower in patients with a higher baseline risk/higher baseline cholesterol level.
Let’s say that you could use an intervention that could delay death, by a few to several years, in one out of 50 patients subjected to it. Is there a threshold in terms of monetary expenses above which you think this intervention should not be offered (assuming it is covered by insurance)? Click here to submit your answer via MetaClinician and see what your peers would do.
 English
English
 Español
Español
 українська
українська