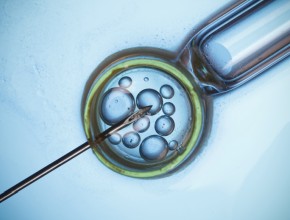
US recommendations for nonalcoholic liver disease
Chalasani N, Younossi Z, Lavine JE, et al. The diagnosis and management of nonalcoholic fatty liver disease: Practice guidance from the American Association for the Study of Liver Diseases. Hepatology. 2018 Jan;67(1):328-357. doi: 10.1002/hep.29367. Epub 2017 Sep 29. Review. PubMed PMID: 28714183.
Related guidelines and other resources
Fibrosis 4 Score. GIHep. http://gihep.com/calculators/hepatology/fibrosis-4-score/. Accessed January 17, 2019.NAFLD Fibrosis Score. GIHep. http://gihep.com/calculators/hepatology/nafld-fibrosis-score/. Accessed January 17, 2019.
National Institute for Health and Care Excellence. Non-alcoholic fatty liver disease (NAFLD): assessment and management. https://www.nice.org.uk/guidance/ng49. Published July 6, 2016. Accessed January 17, 2019.
European Association for the Study of the Liver (EASL); European Association for the Study of Diabetes (EASD); European Association for the Study of Obesity (EASO). EASL-EASD-EASO Clinical Practice Guidelines for the management of non-alcoholic fatty liver disease. Diabetologia. 2016 Jun;59(6):1121-40. doi: 10.1007/s00125-016-3902-y. PubMed PMID: 27053230.
Different practice guidelines give (slightly) different recommendations for the management of nonalcoholic fatty liver disease (NAFLD).
This paper summarizes a recent guidance document by the American Association for the Study of Liver Diseases (AASLD). NAFLD has an estimated prevalence of 25% and is strongly associated with dyslipidemia, diabetes, and obesity. Inflammation and injury of the liver (nonalcoholic steatohepatitis, or NASH) occurs in about 5% of patients with NAFLD and may lead to cirrhosis and hepatocellular carcinoma. With treatment now available for hepatitis C, NASH is becoming the leading cause of liver transplantation.
The AASLD recommends against active screening for NAFLD, arguing that the long-term consequences of treatment (especially pharmacologic) are not clear. It recommends that the first strategy among people with incidentally detected NAFLD should be the assessment and modification of risk factors (diabetes, hyperlipidemia, obesity). Alcohol intake should obviously be considered.
The risk of progression to fibrosis may be assessed using the fibrosis-4 (FIB-4) test (taking into account age, platelet count, aspartate aminotransferase [AST], and alanine aminotransferase [ALT]; see FIB-4 index at www.mdcalc.com) and the NAFLD score (additionally taking into account body mass index and albumin level; see NAFLD score at www.mdcalc.com) as well as liver elastography.
Treatment options include weight loss (NASH may stabilize with a weight loss of about 5%; all histologic features may improve with a loss of 10%). According to the AASLD, pioglitazone and vitamin E—although recommended by some clinical practice guidelines, such as the ones by the National Institute for Health and Care Excellence (NICE)—should be limited to patients without diabetes and with biopsy-proven NASH. Of note, NICE and other European guidelines recommend screening (eg, of people aged >50 years with metabolic syndrome).
You have diagnosed your patient with nonalcoholic steatohepatitis. Exploring potential treatment, you found both European and North American practice guidelines. They address the importance of weight loss, limiting alcohol consumption, diabetes, and lipid control. Which guideline is more open to recommend treatment with vitamin E (400-800 U/day) and/or pioglitazone? Click here to submit your answer via MetaClinician and see your peers’ responses.
Lifetime risk of stroke
Approximately 1 in 4 people will develop stroke during their lifetime!
This report used data from the Global Burden of Disease (GBD) study and estimated the cumulative lifetime risk of stroke among people aged ≥25 years. The analysis was adjusted for competing causes of death (ie, in a country with high and early nonstroke mortality, the probability of developing stroke was expected to be lower).
The estimated total lifetime risk of stroke from the age of 25 onward was about 25% for both men and women, with about two-thirds of strokes being ischemic and one-third being hemorrhagic. The highest risk was present in East Asia (39%) and Central/Eastern Europe (32%). The greatest risk among men was in China (41%) and among women in Latvia (42%). The risk in sub-Saharan Africa was lowest (12%) but it increased to 22% after taking into account the competing causes of death (ie, the relatively shorter life-span).
Your new patient is admitted to the hospital with a diagnosis of stroke. His family asks you how common stroke is. Click here to submit your answer via MetaClinician and see your peers’ responses.
US health-care spending
Bauchner H, Fontanarosa PB. Health Care Spending in the United States Compared With 10 Other High-Income Countries: What Uwe Reinhardt Might Have Said. JAMA. 2018 Mar 13;319(10):990-992. doi: 10.1001/jama.2018.1879. PubMed PMID: 29536083.
Emanuel EJ. The Real Cost of the US Health Care System. JAMA. 2018 Mar 13;319(10):983-985. doi: 10.1001/jama.2018.1151. PubMed PMID: 29536081.
Anderson GF, Reinhardt UE, Hussey PS, Petrosyan V. It's the prices, stupid: why the United States is so different from other countries. Health Aff (Millwood). 2003 May-Jun;22(3):89-105. PubMed PMID: 12757275.
US health-care spending is markedly higher than in other high-income countries. It’s the prices, stupid!
In this analysis, the authors report that in 2016 the United States spent 17.8% of its gross domestic product (GDP) on health care compared with expenditures ranging from 9.6% in Australia up to 12.4% in Switzerland. This occurred despite about 10% of the total US population not having active insurance and most health indices at the bottom of the analyzed list of countries: for example, the lowest life expectancy and the highest infant mortality rate.
Investigating reasons for the higher costs, this publication and the accompanying editorials quote the famous explanation attributed to Uwe Reinhardt, the economic analysis guru: “It’s the prices, stupid!” For example, the average yearly per-capita cost of medications was $1443 in the United States versus a range from $466 to $939 in other countries. Physicians’ salaries are 30% to 100% higher in the United States, but as there are relatively fewer physicians, the total physician cost per capita is more comparable (eg, $712 in the United States, $693 in Germany, $536 in the Netherlands, $397 in Sweden). Markedly higher use of diagnostic tests accounts in part for the difference (per-capita cost of computed tomography and magnetic resonance imaging is $355 in the United States vs $47 in the Netherlands). The US administration cost of $752 per capita is not only higher than the total cost of physicians but also 3 to 5 times higher than the cost of administration in other countries.
What is the relationship between the estimated per-capita cost of medications versus insurance administration versus physicians’ services in the United States compared with the Netherlands? Click here to submit your answer via MetaClinician and see your peers’ responses.
 English
English
 Español
Español
 українська
українська